Marc Darrow, MD, JD.
When someone contacts our office and they tell us that they have been diagnosed with Post Laminectomy Syndrome we have to get information from them that will allow us to make a realistic assessment if they are someone that we can help. We can help some people with Post Laminectomy Syndrome, we may not be able to help others. How do we know who we may be able to help? We talk to people on the phone, we discuss their pain and symptoms and what happened after the surgery. If we think we can help someone, we tell them to come in for a consultation. If we do not think we can help, we don’t.
Many people who have this procedure get it done only to find out they really did not have a nerve impingement
Many people try to avoid surgery. They spend years in pain, using treatments that usually don’t work but they keep using them. Finally the surgeon and probably their family finally got this person to consent to a laminectomy. A laminectomy removes part of the bone or the lamina from the suspected pain generating area of the spine. Sometimes removing the bone pressing on the nerve is successful. Sometimes it is not successful and the person still has pain. Why? Many people who have this procedure get it done only to find out they really did not have a nerve impingement. I have seen many patients like this. The MRI showed one thing, impingement/herniation, but that was not the source of the pain. The surgeons wound up treating the MRI. So many times people come in to visit us and they had a laminectomy or a fusion in their back, and I ask, “did the doctor ever touch you? Do a physical examination? No, they didn’t touch me. They showed me the MRI and showed me what the problem was.
Are MRIs sending people to back surgery who may not need back surgery?
I want to turn this article over to the surgeons so they can explain how a patient may develop Post Laminectomy Syndrome. This first study was published in the medical publication Biomed Central research notes.(1) It comes from the Anesthesiology, Pain and Palliative Care Department, Federal University of Maranhao in Brazil. These are their observations:
Although not well known, post-laminectomy syndrome is an important cause of chronic back pain, which may lead to decreased quality of life, disability and psychological disorders. The prevalence of post-laminectomy pain was 60 % (in this study group). Most of the patients assessed in this study were male. . . their mean age was 45 years. All of the patients presented with chronic, intense pain that had lasted an average of 7.22 years. None of the patients exhibited high levels of physical fitness.
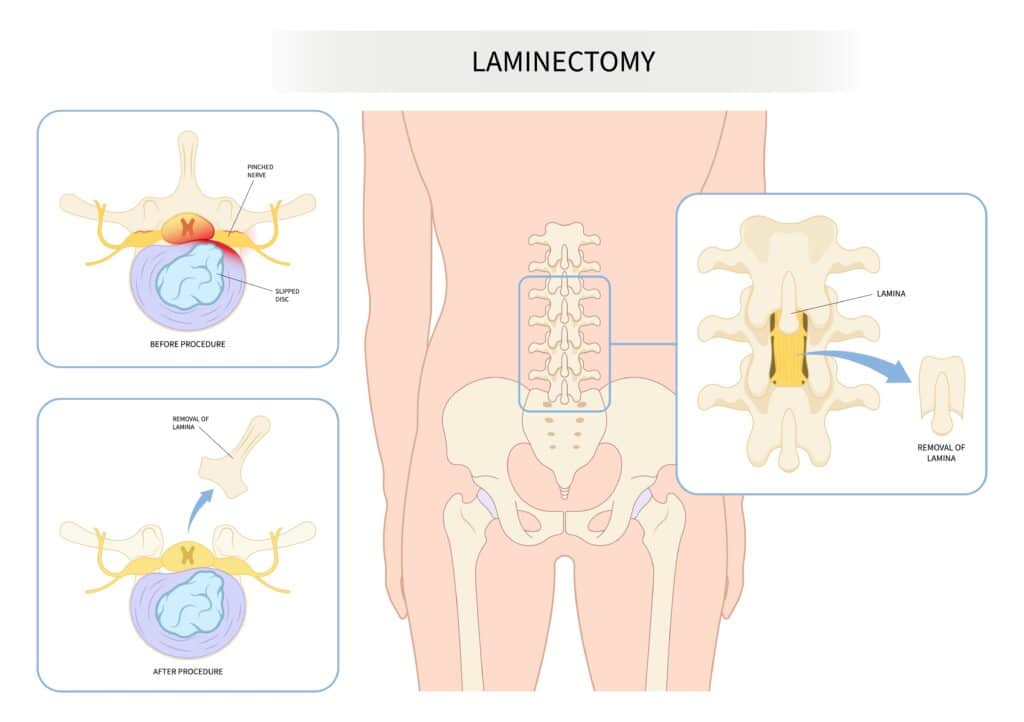
“the surgical procedure is required in only 1–3 % of cases.”
Lumbar laminectomy is one of the surgical procedures used to treat intervertebral disc protrusions (a bulging or herniated disc). It consists of removing the vertebral lamina to expose and allow access to the disc that is responsible for the nerve root compression. Although the vast majority of lumbar sciatic pain is mechanical in nature, the surgical procedure is required in only 1–3 % of cases.
Why does this surgery fail? According to the surgeons:
“The surgery to correct disc herniations is most commonly performed as an elective procedure in the patients who fail conservative treatment and who experience worsening of their lower limb pain and disability. Studies indicate that the failure of herniated-disc surgeries is related to insufficient diagnoses and the incorrect selection of patients for these procedures.
Other reasons? Reserachers ask “Is post-laminectomy syndrome a result of the patient causing failure or the surgeon?”
An October 2021 study (2) wrote: “The etiology of post-laminectomy syndrome can be examined in two groups as factors related to the patient and surgical procedure. Patient diagnoses such as anxiety, depression, somatization disorder, and poor management of pre-operative pain reduce the rate of surgical success. Insufficient decompression or the opposite aggressive surgical approaches are both included in the etiology of post-laminectomy syndrome. Incorrect placement of the graft or screw can cause nerve damage and adhesions and lead to post-operative radicular and neuropathic pain.”
“20–40 % of the patients undergoing lumbar surgery will not experience benefits from the procedure and that the condition will worsen in 1–10 %.”
As many as one-third of the patients undergoing surgery for the correction of lumbar disc conditions experience recurrent postoperative symptoms. (One study states that “20–40 % of the patients undergoing lumbar surgery will not experience benefits from the procedure and that the condition will worsen in 1–10 %.”
The high prevalence in (this) study was perhaps due to inaccurate indications for surgery, in which the preoperative pain may have been attributed to disc herniations despite the other possible differential diagnoses. The main causes of Post Laminectomy Syndrome are foraminal stenosis, internal disc extrusion, pseudoarthrosis and neuropathic pain, which in combination account for more than 70 % of the cases.
Several (studies) have suggested that the misinterpretation that a herniated disc is causing low back pain is the most common reason behind the spinal surgeries that result in post-laminectomy chronic pain syndrome beginning immediately after the procedures. This misinterpretation may be partially caused by an overestimation of the anatomical findings that are revealed during the imaging evaluations but are not related to the lumbago and usually do not explain the pain or justify surgical intervention.”
What more can you say?
- There is a rush to surgery that is not needed.
- Many people who get the surgery are not good candidates for the surgery.
- There was an over-estimation of damage that was thought to be revealed on MRI that were later found out not to be the contributing factor of that person’s pain.
Adjacent segment disease
An April 2024 paper (3) examined patients who had a laminectomy at an unfused level adjacent to an instrumented fusion and if that surgery increases the risk of adjacent segment disease (ASD).
- 789 patients underwent instrumented lumbar fusion and laminectomy at the same level(s) (676 patients) or with an additional adjacent level laminectomy (113 patients) with a minimum of 2-year follow-up.
- Diagnoses were degenerative spondylosis (241 patients), degenerative spondylolisthesis (485 patients) and isthmic spondylolisthesis (63 patients) in addition to central stenosis.
The adjacent laminectomy group developed adjacent segment disease at a significantly greater rate of 57.5% compared with 35.2% of the non-adjacent laminectomy group. Revision surgery rate was also greater in the adjacent laminectomy group (22.1% v 13.5%).
Conclusion: Surgeons should be cautious when performing a laminectomy adjacent to an instrumented fusion, as this increases the rate of adjacent segment disease as well as revision surgery.
Opioid use disorder complicates surgery in the short-term
A June 2022 study (4) examined opioid use disorder (opioid abuse) on postoperative outcomes in patients undergoing primary lumbar laminectomy. The study found patients with opioid use disorder undergoing lumbar laminectomy had significantly longer hospital stays (3.68 vs 1.13 days). Readmission rates were significantly higher (14.57% vs 7.39%) in patients who had an opioid use disorder.
Treatments options after the patient has been diagnosed with Post-Laminectomy Syndrome
The treatment options for the patient with Post-Laminectomy Syndrome is typically limited to more surgery or pain management.
- Some people may find success with the implantation of a spinal cord stimulation device. Other may not get any benefit and others may see a gradual decline in the pain management benefit that their device has offered them over time. Both of these reasons lead to a surgical removal of the device.
- Some patients may find themselves managed with opioid medications because there is thought to be no other way. Prescription narcotic use is a challenging way to manage pain.
- Some patients may be enrolled in exercise or physical therapy programs which will try to convince the body, through muscle education, how to function without causing pain.
- Some patients may require coping strategies and counselling.
A study from the Mayo Clinic published in 2018 (5) suggested a combination of all these treatments may help post-laminectomy syndrome patients who have previously undergone spinal cord stimulation and failed.
For some people physical therapy may help, but even that is debated. A 2019 study (6) wrote: “Persistent post-surgical pain is a common condition following surgery, resulting in persistent pain and reduced quality of life. While pharmacological management is common, its effectiveness remains equivocal. . . Due to ongoing challenges in the management of Persistent post-surgical pain alternate treatment strategies such as physiotherapy are being trailed. Despite a number of methodological constraints, current evidence indicates that physiotherapy could play a role in the management of Persistent post-surgical pain.”
Spinal cord stimulation (SCS) implantation’s questionable benefits in post laminectomy syndrome.
A January 2022 paper (7) examined the successes and failures of spinal cord stimulation for post laminectomy syndrome and why patients would need opioids following spinal cord stimulation (SCS) implantation.
This is a large study of 26, 179 with post laminectomy syndrome patients who received an SCS implant. The average patient age was 60.
- Compared with those who did not receive an SCS, individuals who received an SCS were more likely to be using and average of 4.3 opioid prescriptions preimplantation prescriptions but less likely to be using opioids after SCS implantation against a control group. BUT not by much. After SCS implantation average of 3.8 opioid prescriptions in the SCS group compared to 4 opioid prescriptions in the control; group. The conclusion here: “findings suggest that under real-life conditions, SCS was associated with small, clinically questionable associations with opioid discontinuation and not starting opioids in the context of post laminectomy syndrome.
Can Bone Marrow Stem Cell Injections Help Post Laminectomy Syndrome?
The above study describes various coping mechanisms for dealing with Post-Laminectomy Syndrome because there is thought to be no other answers. Sometimes people presented with these options call or email us because they want to know if bone marrow derived stem cell injections can help them heal.
The main considerations of why the patient continues to suffer from back pain after this procedure is two fold. The surgery did not address the true cause of the patient’s pain. The surgery itself caused more pain by damaging structures.
Recurring disc herniation and stenosis
If the patient continues to have recurring disc herniation, stem cell therapy may help by addressing the possible cause of the disc herniation.
- Disc herniation can be caused by injured ligaments and tendon attachments to the bone. Realistically, pain after surgery can find its source in the same pain generators that were activating before the surgery, the abnormal or hypermobility of the vertebrae.
- If the ligaments and tendons of the spine are loose, the vertebrae can cause compression throughout the spine. It is possible that the laminectomy may have found one source of the pain, but not all the sources of the pain. Further, as the spine continues to suffer from degenerative disc disease, more vertebrae will start moving around. It may be at this time a fusion would be recommended to a patient already suspicious of more surgery.
The ligaments which hold the vertebrae to each other may have been the cause of the patient’s pain all along and the continued cause of pain after the procedure. Laminectomy does not address ligament damage nor does MRI see it.
Tendon and Muscle damage
Stem cell therapy may help if there is a situation of tendon and muscle damage. In a situation like this we would examine the spine and look for tenderness and weakness in the muscle attachments / tendons and the spinal ligaments. If these structures are damaged, they may be treated with regenerative injections including Platelet rich plasma therapy and/or stem cell therapy.
There has to be a realistic expectation of what these treatments can do and what they can’t do. If there are issues of continued pain following a surgery, stem cells and PRP treatments may be effective in helping pain if there are issues with ligament and tendon instability causing spinal instability. Stem cells and PRP may help strengthen the tendon/muscle attachments and help patients who suffer from continued spasms.
Platelet Rich Plasma injections
- PRP treatments involve collecting a small amount of your blood and spinning it in a centrifuge to separate the platelets from the red cells. The collected platelets are then injected back into the injured area to stimulate healing and regeneration. Research has shown PRP to be effective in treating degenerative disc disease by addressing the problems of cervical spine ligament instability.
Stem cell injections
- Stem cell injections help restore ligaments strength by causing the regeneration of ligament, tendon, cartilage and bone regeneration.
These treatments do not work for everyone.
Summary
I’ve had several patients who came in with central back pain, that is pain right above the buttocks on the pelvis, and the low middle of their back. They had a back surgery and the back surgery made their condition worse because the surgery addresses something that wasn’t the problem. Most of those issues we see in patients with back pain are ligament sprains. Ligaments hold the vertebrae together. If you suffer from Post-Laminectomy Syndrome, stem cell therapy may be able to help. Please use the form below and send in an email to me.
Call for a free phone consultation with our staff 800-300-9300
Related articles
Failed Back Surgery Syndrome: Conservative care, Spinal Cord Stimulators
References:
1 Garcia JB, Rodrigues DP, Leite DR, do Nascimento Câmara S, da Silva Martins K, de Moraes ÉB. Clinical evaluation of the post-laminectomy syndrome in public hospitals in the city of São Luís, Brazil. BMC research notes. 2015 Dec;8(1):1-7.
2 Akkemik Ü, Onay M, Güleç MS. Effectiveness of interventional procedures for post-laminectomy syndrome: A retrospective study. Agri: Agri (Algoloji) Dernegi’nin Yayin Organidir= The Journal of the Turkish Society of Algology. 2021 Oct 1;33(4):253-60.
3 Simonetta B, Adeniyi B, Corbett A, Crandall D, Chang M. LAMINECTOMY ADJACENT TO INSTRUMENTED FUSION INCREASES ADJACENT SEGMENT DISEASE. Spine. 2024 Apr 10:10-97.
4 Idrizi A, Paracha N, Lam AW, Gordon AM, Saleh A, Razi AE. Association of Opioid Use Disorder on Postoperative Outcomes Following Lumbar Laminectomy: A Nationwide Retrospective Analysis of the Medicare Population. International Journal of Spine Surgery. 2022 Jun 28.
5 Bailey JC, Kurklinsky S, Sletten CD, Osborne MD. The effectiveness of an intensive interdisciplinary pain rehabilitation program in the treatment of post-laminectomy syndrome in patients who have failed spinal cord stimulation. Pain medicine. 2018 Feb 1;19(2):385-92.
6 Robinson A, McIntosh J, Peberdy H, Wishart D, Brown G, Pope H, Kumar S. The effectiveness of physiotherapy interventions on pain and quality of life in adults with persistent post-surgical pain compared to usual care: A systematic review. PloS one. 2019 Dec 13;14(12):e0226227.
7 Vu TN, Khunsriraksakul C, Vorobeychik Y, Liu A, Sauteraud R, Shenoy G, Liu DJ, Cohen SP. Association of Spinal Cord Stimulator Implantation With Persistent Opioid Use in Patients With Postlaminectomy Syndrome. JAMA network open. 2022 Jan 4;5(1):e2145876-.






