Many people email us about their hip and back pain. Some have been recommended to a hip replacement, some have been recommended to a spinal surgery. Some have been recommended to both surgeries and they are in the process of choosing between one or the other and exploring options to help them avoid one or the other surgery, even both.
Back surgery? Hip Surgery? Do you need either? Both? Neither?
The problem of hip-spine complex pain is that it is indeed a complex problem of hip and spine pain. As we will see in the research below, problems of the hip / spine may lead some people to get a back surgery for a hip problem and a hip surgery for a back problem. Doctors have noted that the symptoms of hip arthritis pain and spinal stenosis leg pain can be very similar, with only subtle differences in both history and clinical physical examinations. Spinal stenosis is classically diagnosed in patients with leg pain that occurs during standing or walking and is relieved when the individual sits down.
A May 2024 paper in the medical journal Arthroscopy (1) writes: “Low back pain present concurrently with hip impingement or labral pathology is frustrating for both patient and surgeon. It is difficult to distinguish true hip pathology from secondary low back symptoms, even with the use of diagnostic injections, cross-sectional imaging, electromyography, and/or nerve conduction studies.”
This research centers on arthroscopy repair, less invasive than hip replacement, but still just as problematic to the decision between the possible cause of pain. Is it the hip or spine?
A July 2021 editorial (2) repeats the confusing problem of true pain diagnosis and which surgery should go first. “Several studies have reported that patients with a previous lumbar arthrodesis (fusion) undergoing hip replacement have lower patient-reported outcomes and greater revision rates compared with patients without previous lumbar surgery, and similar to its effect on outcomes after hip replacement, lumbar spine disease can compromise outcomes after hip arthroscopy. On the other side of the coin, replacement has been shown to improve low back pain in patients with concomitant hip osteoarthritis.”
Research: The question of which to have surgery on first, the hip or the spine, is much more complex and risky than thought
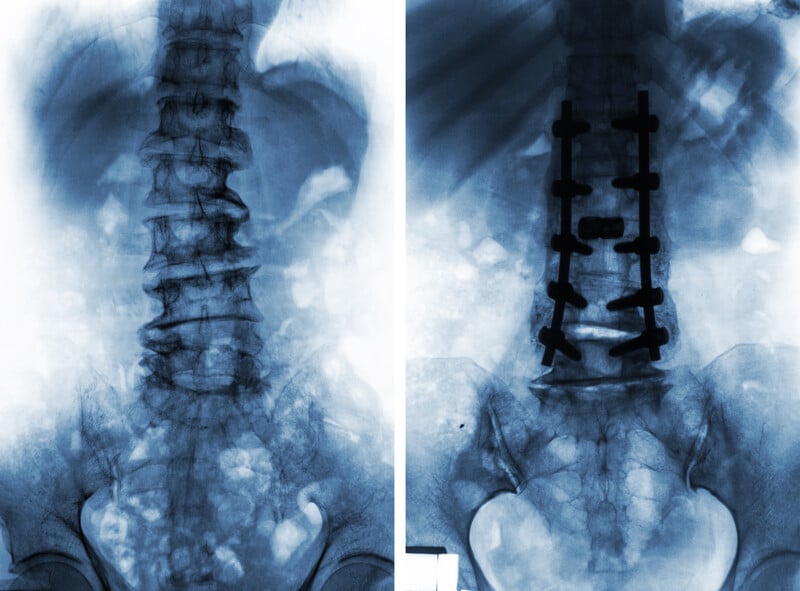
The option to have lumbar spinal surgery and hip replacement at the same time is clearly one that is not recommended for obvious reasons. So a decision has to be made. Spinal surgery or hip replacement surgery? One has to come first and one has to wait.
At Washington University School of Medicine, Departments of Orthopaedic Surgery and Neurology and Physical Therapy, surgeons and therapists wanted to examine patients who had hip osteoarthritis and back pain. The hip-spine complex can be a tricky and complex area to diagnose. Finding the true source or sources generating a patient’s pain can be equally complex. This makes the first surgery decision even more difficult.
In this study, the hip was the true disguised pain generator in back pain patients
In their 2018 study presented in the journal PMR, (3) the Washington University team found links between the hip and the spine affecting pain and function. The key finding was that hip disease, before it was even evident on an MRI as osteoarthritis, could cause problems in the lower back. The hip was the true disguised pain generator in back pain patients.
- What is this research telling us? If you had an MRI of your hip, and nothing presented itself as obvious, then the doctor may chase something in the spine that is not causing the pain. You may get a back surgery that you did even need.
Research: A patient presenting with low back pain should be examined for hip osteoarthritis
The same team of researchers, publishing research earlier in March 2017 (4) were also able to conclude that physical examination findings indicating hip osteoarthritis (loss of range of motion and acute pain) are common in patients who also have low back pain. A patient presenting with low back pain should be examined for hip osteoarthritis.
Research: Source of pain location confusion: Is it from inside the hip joint, outside the hip joint, is it from lumbar stenosis?
Similar findings were reported in a study from doctors at Vanderbilt Orthopaedic Institute (5) the incidence of symptomatic osteoarthritis of the hip and degenerative lumbar spinal stenosis were examined because the subjective complaints can be similar, and it is often difficult to differentiate intra- and extra-articular hip pathology from degenerative lumbar spinal stenosis. These conditions can present concurrently, which makes it challenging to determine the predominant underlying pain generator. A thorough history and physical examination, coupled with selective diagnostic testing, can be performed to differentiate between these clinical entities and help prioritize management.
It should be noted that a physical examination was called for. In the above study “selective diagnostic testing.”
Hip or spine surgery first? Research says there is confusion and controversy even among the most experienced surgeons
Because you cannot do a spinal surgery and a hip replacement at the same time the patient and their surgeons need to pick the one that helps the most. If you went to your hip surgeon, he/she may recommend the hip first, if you went to your spinal surgeon he/she may recommend spinal surgery first. So you have 2 different “first surgery,” recommendations. Sometimes, there is agreement, sometimes there is conflicting opinions.
A June 2019 published in the Bone and joint journal (6) suggests controversy in the decision making process of the patient with hip and spinal degenerative disease. Here is what the surgeons are struggling with.
- Patients who are being recommended to both hip replacement and lumbar spinal surgery have to make a choice which surgery to do first. Recommendations from their surgeons as to which surgery should be performed first remain uncertain and can confuse the patient.
A survey of hip and spinal surgeons asked the question: “When do you do the hip replacement first?” In all 88, surgeons, 51 hip surgeons and 37 spinal surgeons were asked.Here is how the survey went
First case: Patient has painful hip osteoarthritis and lumbar spinal stenosis with neurological claudication. (Pain radiating into the legs caused by a “pinched, inflamed nerve.”
- Hip surgeons: 59% say do the hip first
- Spinal surgeons 49% say do the hip first
Second case: Patient has painful hip osteoarthritis and lumbar degenerative spondylolisthesis (slipped disc) with leg pain
- Hip surgeons: 73% say do the hip first
- Spinal surgeons 70% say do the hip first
Third case: Patient has painful hip osteoarthritis and lumbar disc herniation with leg weakness
- Hip surgeons: 47% say do the hip first
- Spinal surgeons 19% say do the hip first
Fourth case: Patient has painful hip osteoarthritis and lumbar scoliosis with back pain
- Hip surgeons: 47% say do the hip first
- Spinal surgeons 78% say do the hip first
Fifth case: Patient has painful hip osteoarthritis and thoracolumbar disc herniation with myelopathy (spinal cord pressure).
- Hip surgeons: 0% say do the hip first
- Spinal surgeons: 0% say do the hip first
In only one scenario, spinal cord compression, is there 100% agreement.
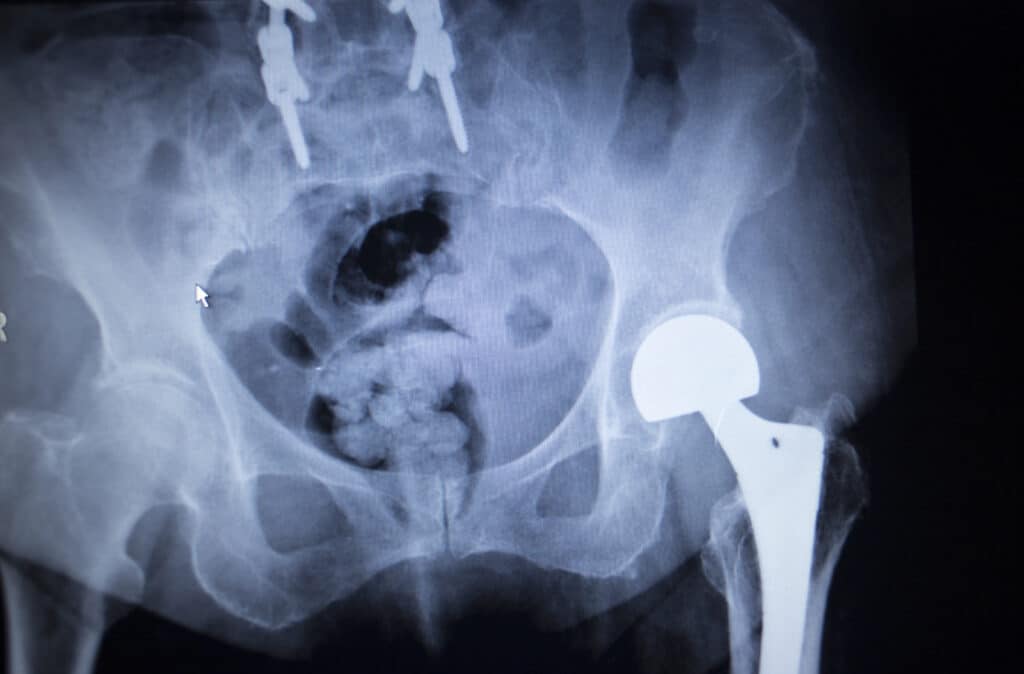
In my article Are MRIs sending people to unnecessary spinal surgery? I discuss the documented problems of spinal MRIs sending people to a surgery they do not need. Here are some of the highlights of that article:
- A study that appeared in the medical journal Radiologia (Radiology) (7) where researchers had concerns about the enthusiasm some surgeons had for surgery that was likely inappropriate.
This is from the study:
- Most imaging findings (Scans and MRIs), find degenerative changes that reflect anatomic peculiarities or the normal aging process and turn out to be clinically irrelevant.
- Imaging tests have proven useful only when systemic disease is suspected or when surgery is indicated for persistent spinal cord or nerve root compression.
- Many treatments (surgeries) have proven inefficacious, and some have proven counterproductive, but they continue to be prescribed because patients want them and there are financial incentives for doing them.”
The keywords of the research are “ineffective,” and “counterproductive,” for the patient.
Below is research that appeared in the Annals of the New York Academy of Sciences (8):
Summary findings:
- Numerous imaging studies (MRIs and Scans) have attempted to determine a definitive association between Intervertebral disc degeneration (Degenerative disc disease) and low back pain.- However, disc degeneration is not a sufficient diagnosis for pain development, as evidenced by large numbers of asymptomatic patients with abnormal findings on MRI or CT.
- Using MRI, Intervertebral disc herniations are seen in 22–67% of asymptomatic adults and spinal stenosis in 21% of asymptomatic adults over 60, and CT evidence of spinal facet joint osteoarthritis was shown to have no correlation with low back pain. Abnormal findings on MRI scans were not predictive of the development or duration of low back pain.
Do not assume your pain is coming from what the MRI shows you. Your pain may not be captured on this film.
In a study published in the Journal of Neurosurgery, Spine (9) that examined patients with back pain, investigators found that patients in fact did expect to get an MRI when they have back pain and that the MRI will reveal exactly what the cause of their pain is. Not only that but:
- more than 50% of the patients would have a spinal surgery if their doctor told them they had an abnormal spinal MRI, even if they had no pain or restricted movement.
- “Patients overemphasize the value of radiological studies and have mixed perceptions of the relative risk and effectiveness of surgical intervention compared with more conservative management.”
In 2022 (10) researchers questioned why many patients with low back pain with or without radiculopathy commonly undergo magnetic resonance imaging (MRI) for diagnosis and therapeutic assessment, yet the final intervention is mainly centered around nonoperative treatment. Therefore they questioned: “the value of MRI in patients with low back pain with or without radiculopathy.” What their study showed was low back pain patients with leg weakness are prone to receiving surgical treatments after pharmacological treatments, while additional MRI seemed to add limited value to the outcome prediction of low back pain patients. Therefore, for LBP patients whose clinical baseline characteristics suggest a low risk for receiving surgical treatment, advanced imaging examinations should not be routinely prescribed.
In our practice we often see patients who have severe back pain and carry with them an MRI, X-ray and/or scan that are inconclusive. Doctors writing in the European Journal of Pain agree and say while controversial, research supporting MRI use do not permit definite conclusions.(11) This supports recent findings that say despite doctors frequently requesting MRIs for the lumbar spine, sometimes for weak or various reasons, that imaging performs poorly and it is not likely to identify the anatomical structures that are the source of pain.(12)
Perhaps this is why hip surgery is more routinely recommended first form any back pain patients
Having unnecessary surgery, it happens quite often, especially when the hip is involved.
In a study published in the medical journal Modern Rheumatology, (13) surgeons discussed the complexity of hip disease and how it impacts other joints and areas of the body.
Here the surgeons found that:
- Hip disease was the cause of knee pain in 29 % of patients.
- Hip disease was the cause of low back pain in 17 % of patients.
Their warning to their fellow surgeons?
- “be aware of hip disease masquerading as knee pain or low back pain” That is how wrong surgeries may be performed.
Here is study from surgeons in the United Kingdom. Published in the medical journal International Orthopaedics, (14) the surgical team of this study wanted to answer the question as to why up to 20% of total knee replacement patients complain of persisting pain after the knee replacement. Here was there answer:
The investigators examined 45 consecutive patients with pain after total knee replacement. Of the 45 patients, one-third, 15 patients had degenerative hip and lumbar spine disease. Nine patients had unexplained pain.
The study concluded: “Patients may still be undergoing knee arthroplasty for degenerative lumbar spine and hip osteoarthritis. We suggest heightened awareness at pre- and post-operative assessment and thorough history and examination with the use of diagnostic injections to identify the cause of pain if there is doubt.”
Study: Surgical revisions
A March 2024 study (15) sought to add input into the “increasing debate among orthopaedic surgeons over the temporal relationship between lumbar spinal fusion and total hip replacement for patients with hip-spine syndrome.” The researchers noted “few large studies have directly compared the results of patients who undergo lumbar spinal fusion prior to total hip replacement to those who undergo lumbar spinal fusion after total hip arthroplasty.” In a study of 716,000 patients. The researchers found lumbar spinal fusion first patients experienced significantly more postoperative dislocations at 90 days and 1 year compared to hip replacement patients. There were a similar number of revisions performed for spine first and hip first surgery patients at both 90 days and 1 year. At one year, lumbar spinal fusion first patients experienced more pneumonia and joint infection.
A study published in February 2026 (16) looked into the rates of lumbar spine revisions and the complications that occurred after surgery in patients who had both hip osteoarthritis and issues with their lumbar spine. In total, 70,265 patients were included in the study. After five years, the rates of lumbar revisions were found to be 8.6% for those who had lumbar fusion before undergoing total hip arthroplasty, while it was 8.4% for those who had hip arthroplasty before lumbar fusion. When these patients were compared to those who only had lumbar fusion, the chances of needing a lumbar revision were 5.59 times greater for the lumbar fusion before total hip arthroplasty group and 2.61 times greater for the hip arthroplasty before lumbar fusion group.
Non-surgical options
Lumbar spinal stenosis – surgery and injections | Joint Rehab Los Angeles
Call for a free phone consultation with our staff 800-300-9300
References:
1 Scott EJ. Hip Arthroscopy in Patients with Spine Pain: Outcomes Vary Compared to Patients with Isolated Hip Pathology, but Many Hip-Spine Patients Do Just as Well. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2024 May 4.
2 Jimenez AE, Domb BG. Editorial Commentary: Spine pathology may compromise the results of hip arthroscopy: will hip arthroscopy improve low back pain?. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2021 Jul 1;37(7):2110-1.
3 Prather H, Cheng A, May KS, Maheshwari V, VanDillen L. Association of Hip Radiograph Findings with Pain and Function in Patients Presenting with Low Back Pain. PM&R. 2017 Jun 16.
4 Prather H, Cheng A, May KS, Maheshwari V, VanDillen L. Hip and Lumbar Spine Physical Examination Findings in People Presenting With Low Back Pain With or Without Lower Extremity Pain. J Orthop Sports Phys Ther. 2017 Feb 3:1-36. doi: 10.2519/jospt.2017.6567.
5 Liu N, Goodman SB, Lachiewicz PF, Wood KB. Hip or spine surgery first?: a survey of treatment order for patients with concurrent degenerative hip and spinal disorders. Bone Joint J. 2019 Jun;101-B(6_Supple_B):37-44. doi: 10.1302/0301-620X.101B6.BJJ-2018-1073.R1. PubMed PMID: 31146559; PubMed Central PMCID: PMC6568023.
6 Devin CJ, McCullough KA, Morris BJ, Yates AJ, Kang JD. Hip-spine syndrome. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2012 Jul 1;20(7):434-42.
7 Kovacs FM, Arana E. Degenerative disease of the lumbar spine. Radiologia. 2016 Apr;58 Suppl 1:26-34. doi: 10.1016/j.rx.2015.12.004. Epub 2016 Feb 10
8 Mosley GE, Evashwick‐Rogler TW, Lai A, Iatridis JC. Looking beyond the intervertebral disc: the need for behavioral assays in models of discogenic pain. Annals of the New York Academy of Sciences. 2017 Aug 10.
9 Franz EW, Bentley JN, Yee PP, Chang KW, Kendall-Thomas J, Park P, Yang LJ. Patient misconceptions concerning lumbar spondylosis diagnosis and treatment. J Neurosurg Spine. 2015 May;22(5):496-502. doi: 10.3171/2014.10.SPINE14537. Epub 2015 Feb 27.
10 Wang H, Liu C, Meng Z, Zhou W, Chen T, Zhang K, Wu A. Real-world study for identifying the predictive factors of surgical intervention and the value of magnetic resonance imaging in patients with low back pain. Quantitative Imaging in Medicine and Surgery. 2022 Mar;12(3):1830.
11 Steffens D, Hancock MJ, Maher CG, Williams C, Jensen TS, Latimer J. Does magnetic resonance imaging predict future low back pain? A systematic review. Eur J Pain. 2013 Nov 26. doi: 10.1002/j.1532-2149.2013.00427.x. [Epub ahead of print]
12 Balagué F, Dudler J. [Imaging in low back pain: limits and reflexions]. Rev Med Suisse. 2013 Jun 26;9(392):1351-2, 1354-6, 1358-9
13 Nakamura J, Oinuma K, Ohtori S, et al. Distribution of hip pain in osteoarthritis patients secondary to developmental dysplasia of the hip. Mod Rheumatol. 2012 Apr 11
14 Al-Hadithy N, Rozati H, Sewell MD, Dodds AL, Brooks P, Chatoo M. Causes of a painful total knee arthroplasty. Are patients still receiving total knee arthroplasty for extrinsic pathologies? Int Orthop. 2012 Jan 11.
15 Mohamed NS, Salib CG, Sax OC, Remily EA, Douglas SJ, Delanois RE. Spinal fusion and total hip arthroplasty: why timing is important. Hip International. 2024 Mar;34(2):174-80.
16 Ambreen Y, Veliky C, Ibrahim MT, Kuttner N, Yu E. Total hip arthroplasty increases the odds of revision in lumbar fusion: a national cohort study. Asian Spine J. 2026 Feb 11.






