Marc Darrow, MD, JD
Most of the people that contact our office looking for treatment for their thumb pain have already had a long history of treatments with limited success. In fact, many will confess that their doctors are now recommending pain management (anti-inflammatories and painkillers) as their primary treatments now that splints, physical therapy, and a generous amount of ice are no longer helping. These people will receive pain management until the decision is made to go to surgery or “live with it.” For many, the benchmark of when to proceed to surgery is when cortisone injections fail to offer relief and is in fact giving the person more pain.
So what do we do for these bone on bone thumb people who have basically lost the use of the hands because they have no grip strength and are being pain managed? We offer a physical examination, and assessment of their pain and functional challenges, and when appropriate a recommendation for treatment.
Thumb fusion surgery and joint replacement Surgery or no surgery?
Surgery or no surgery?
A June 2024 study (1) explored the long-term changes in pain and hand function over a 2-year period in patients with thumb osteoarthritis. The researchers looked at those who received occupational therapy or brief information on how to manage their thumb pain while waiting for a surgical consultation. When comparing groups receiving occupational therapy only, occupational therapy and surgery, brief information only, and brief information and surgery, patients receiving brief information and surgery had significantly more pain and poorer function at four months compared to the other groups, whereas no difference was found between the four groups at 24 months. (Eventually the occupational; therapy and surgery performed equally).
In patients who received surgery after having received occupational therapy, pain and function did not change between 4 and 24 months, suggesting that surgery did not provide additional improvement in this group.
What the researchers suggested was that a patient’s thumb pain could be managed equally with or without surgery.
A September 2020 study (2) says this: “Resection arthroplasty (a joint replacement where the bones of the thumb may be repositioned at the same time) still is the gold standard for the treatment of basal thumb arthritis. In most patients, satisfactory results can be expected. However, the few patients with persisting problems are a challenge for the hand surgeon. They may complain of neuromas, tendinitis of the flexor carpi radialis (FCR) tendon, impingement and/or proximalization of the first metacarpal, arthritis of the scaphotrapezoidal joint or carpal collapse in the case of pre-existing scapholunate instability.”
Concerns surrounding trapeziometacarpal surgery.
Trapeziometacarpal joint osteoarthritis or rhizarthrosis is degeneration at the trapezium bone at the wrist and the first metacarpal bone of the thumb. The Trapeziometacarpal joint is a tricky joint to repair with surgery. This according to surgeons publishing research in the American Journal of hand surgery (June 2019). The surgeons expressed concerns that failure rates of trapeziometacarpal implants were considered high because of aseptic loosening, dislocation, and persisting pain.(3) This followed an April 2018 study (4) that also questioned whether thumb joint replacement surgery at the trapeziometacarpal joint provided significant benefits for the patient.
A brief look at this study reveals that doctors looked at four women diagnosed with stage III osteoarthritis at the Trapeziometacarpal who underwent total joint replacement surgery.
- What the surgeons found was the surgery was able to restore some thumb function but did not fully replicate the movements of a healthy trapeziometacarpal joint.
A February 2022 paper (5) added: “Until further high-quality research indicates otherwise, simple trapeziectomy should be the preferred surgical modality for base of the thumb arthritis.”
1 Tveter AT, Østerås N, Nossum R, Eide RE, Klokkeide Å, Matre KH, Olsen M, Kjeken I. Long‐term changes in pain and function in patients with thumb base osteoarthritis receiving brief information, occupational therapy and/or surgery. Musculoskeletal Care. 2024 Jun;22(2):e1883.
2 Löw S, Kiesel S, Spies CK. Revision surgery after resection arthroplasty of the thumb saddle joint. Der Orthopade. 2020 Sep 1;49(9):762-70.
3 Ganhewa AD, Wu R, Chae MP, Tobin V, Miller GS, Smith JA, Rozen WM, Hunter-Smith DJ. Failure Rates of Base of Thumb Arthritis Surgery: A Systematic Review. The Journal of hand surgery. 2019 Jun 28.
4 D’Agostino P, Dourthe B, Kerkhof F, Vereecke EE, Stockmans F. Impact of Osteoarthritis and Total Joint Arthroplasty on the Kinematics of the Trapeziometacarpal Joint: A Pilot Study. The Journal of hand surgery. 2018 Apr 1;43(4):382-e1.
5 Challoumas D, Murray E, Ng N, Putti A, Millar N. A Meta-analysis of Surgical Interventions for Base of Thumb Arthritis. Journal of Wrist Surgery. 2022 Feb 23;11(06):550-60.
Hypermobility of the first Carpometacarpal joint is a ligament problem
A May 2022 paper (2) suggested the problem of hypermobility of the first Carpometacarpal joints joint may adversely affect hand function and may lead to osteoarthritis later in life. It presents more commonly in younger women with generalized joint hypermobility or postmenopausal women with early stages of arthritis. It may follow trauma and elective surgical interventions. Clinically, joint subluxation manifests with a prominent and unstable thumb base, and is radiographically confirmed by stress views. A variety of ligament reconstruction techniques are available to stabilize the Carpometacarpal joints joint including open ligament reconstruction.”
Trapeziectomy concerns
Trapeziectomy is the removal of the trapezium bone at the thumb’s base. Why remove a bone, even a small one? Because the bone is thought to be the primary cause of pain as it has become misshapen by osteoarthritis. In the trapeziectomy with LRTI surgery, a ligament reconstruction procedure is also performed to help the thumb function better anatomically. To someone who uses their hands a lot, as in physically demanding work, the recover time of this procedure is 4 to 6 months. If successful.
Why say, if successful? A study in the medical journal Hand.(6)
Here we have a study from doctors at the University of Massachusetts Medical School. In this study the patient charts of 179 patients who had a thumb surgery were examined. Noted is that 21 patients had both thumbs undergo surgery.
The patients in this study had:
- simple trapeziectomy with or without LRTI and with or without Kirschner wire stabilization, or a Weilby procedure. (Tendon reconstruction replaces the void left by the bone removal).
- The average follow-up was 11.6 months
- Seventy hands had a postoperative complication. (That is 70 out of 200 or 35%).
- Ten of these complications were considered major, defined as requiring antibiotics, reoperation, or other aggressive interventions. (That is 5% of all patients).
CONCLUSIONS: Patients undergoing trapeziectomy with LRTI or Weilby had a greater incidence of reported complications when compared with trapeziectomy alone. These results suggest an advantage of simple trapeziectomy.
Why is there a risk that total joint replacement of the Trapeziometacarpal will not reduce pain?
A study from March 2020 (7) suggests that total joint replacement of the trapeziometacarpal joint provides good restoration of the thumb motion and pain relief in most patients. But there is also a risk of no improvement following the operation. The purpose of this study was to identify patients at risk of no clinically important improvement following operative treatment of osteoarthritis of the TMC joint.
- The researchers included 287 consecutive patients (225 women, 62 men) treated with total joint replacement of the trapeziometacarpal joint due to osteoarthritis with an average age of 58.9 years (range 41-80) in a prospective cohort study.
- Looking for who would have the greatest risk for no improvement following the surgery, the researchers found there was an increased risk of no clinically important improvement in hand function for patients with high preoperative grip strength. Also, we found an increased risk of no clinically important improvement in female patients.
But I am young, I need the surgery to get back to work or sport activities
Above we spoke about the realistic 3 – 6 month recovery time that will include splints, medications, therapies. Some doctors believe that the surgical repair of Trapeziometacarpal osteoarthritis is too aggressively recommended and this can lead to unwanted complication.
A study in the journal Hand Surgery and Rehabilitation, (8) suggests:
“The demand for surgical treatment is growing and the patients are becoming younger, adding to the challenge. Surgery can only be proposed after failure of well-conducted conservative treatment and requires a complete X-ray assessment. . . The ideal arthroplasty (joint replacement) technique has yet to be defined but nevertheless, the chosen technique must be well-suited to the patient’s condition. Although many studies have been published on this topic, they do not help us define the treatment indications.
Prospective studies focusing on the patient rather than evaluating a certain surgical technique are needed. Trapeziectomy with or without ligament reconstruction is still considered the gold standard, but the challenges associated with treating its complications limit its indications. Arthrodesis, interposition or arthroplasty are also viable therapeutic options. The patient must be sufficiently informed to be able to contribute to choosing the indication.”
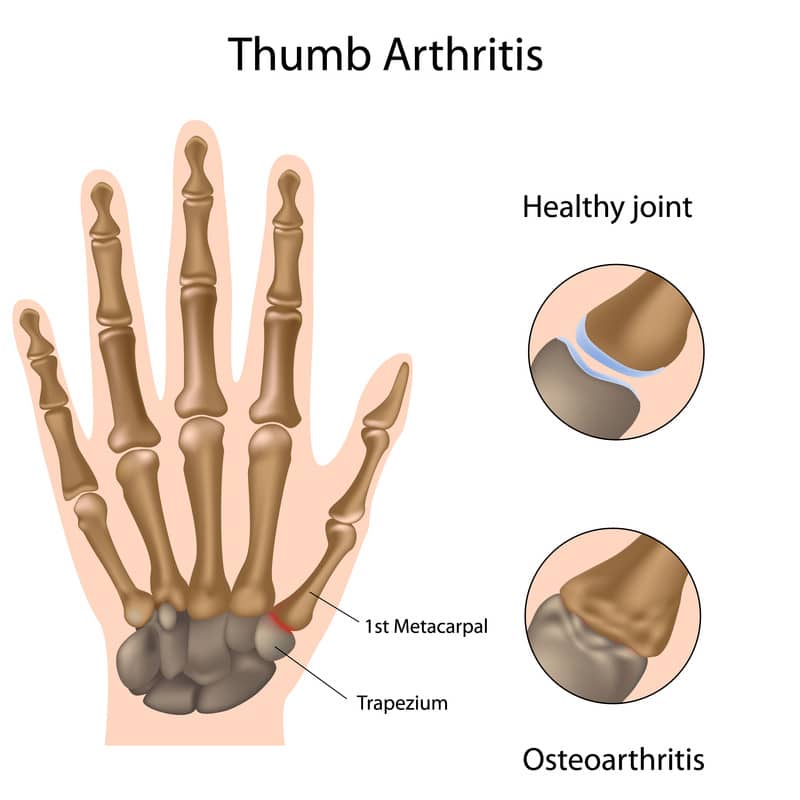
A June 2021 study (9) wrote that thumb surgery is considered when conservative measures fail. The conservative methods listed were ” analgesia, splinting, physiotherapy, and steroid injections.” The primary objective of this study was to assess the safety and effectiveness of the surgical interventions and evaluate whether one surgery was more effective than other.
Effectiveness was measured by reduction in pain, function, range of movement and strength of the joint postoperatively.
The surgeries evaluated were:
- Trapeziectomy – This involves a complete removal of the trapezium bone.
- Trapeziectomy with ligament reconstruction.
- Trapeziectomy with ligament reconstruction and tendon interposition – a tendon is used to fill the space created by the removal of the bone.
- Trapeziectomy with allograft suspension (sometimes amniotic tissue is used to fill the space).
- and joint arthrodesis (fusion surgery).
Which surgery was better? The surgeons wrote: “It is difficult to declare with any degree of certainty which procedure offers the best functional outcome and safety profile. Results suggest Trapeziectomy with ligament reconstruction and tendon interposition. Arthrodesis demonstrated an unacceptably high rate of moderate-severe complications and should be considered with careful consideration.”
Can regenerative medicine injections help you avoid surgery?
People explore these injections as a means to try to avoid surgery. Surgery should always be considered the last option. However, for some people, damage in their thumb joints are so severe and significant that surgery may be the only way. For many others, surgery can realistically be delayed or avoided and the thumb joint repaired with regenerative medicine injections.
PRP injection may help rebuild the thumb joint. A comparison of PRP to cortisone
Above I presented the studies from the surgeons above the challenges they face providing thumb surgery. In this section I will present the options that include Platelet Rich Plasma injections and bone marrow derived stem cell injections.
PRP treatments involve collecting a small amount of your blood and spinning it in a centrifuge to separate the platelets from the red cells. The collected platelets are then injected into the thumb/wrist area to stimulate healing and regeneration. PRP puts specific components in the blood to work. Blood is made up of four main components; plasma, red blood cells, white blood cells, and platelets. Each part plays a role in keeping your body functioning properly. Platelets act as wound and injury healers. They are first on the scene at an injury, clotting to stop any bleeding and immediately helping to regenerate new tissue in the wounded area.
A 2021 study in the journal Cartilage (10) offered this comparison between PRP injections and cortisone injections. Before I start with this study I would like to point out that many people reach out to me and tell me how painful the actual cortisone injection was for them. The problem is the size of the needle and the size of the joint space. When we inject into this area we typically use a freeze spray and very fine needles. This provides the patient with a lot of comfort during the procedure. Also we do not offer a single injection of PRP. We inject into various areas of the wrist and thumb area to maximize the healing effect of the PRP injection.
To the research – the summary learning points:
- Various systematic reviews have recently shown that intra-articular platelet-rich plasma can lead to symptomatic relief of knee osteoarthritis for up to 12 months. There exist limited data on its use in small joints, such as the trapeziometacarpal joint (TMJ) or carpometacarpal joint (CMCJ) of the thumb.
- A prospective, randomized, blind, controlled, clinical trial of 33 patients with clinical and radiographic osteoarthritis of the trapeziometacarpal joint (grades: I-III) was conducted.
- Group A patients (16 patients) received 2 ultrasound-guided IA-PRP injections, while group B patients (17 patients) received 2 ultrasound-guided intra-articular methylprednisolone and lidocaine injections at a 2-week interval.
- Patients were evaluated prior to and at 3 and 12 months after the second injection.
- After 12 months’ follow-up, the IA-PRP treatment has yielded significantly better results in comparison with the corticosteroids, in terms of pain relief, better function, and patients’ satisfaction.
A 2016 study from the University Medical Center Regensburg in Germany (11) evaluated PRP injections into the trapeziometacarpal (TMC) joint. In this report, ten patients TMC joint osteoarthritis were treated with 2 intra-articular PRP injections four weeks apart. Patients were evaluated using Visual Analog Score (0 – 10 pain grading), strength measures, and the Mayo Wrist score (measuring pain intensity and functional status) and DASH (The disabilities of the arm, shoulder and hand score) after 3 and 6 months.
- VAS significantly decreased at six-month follow-up
- The DASH score was unaffected; however, the Mayo Wrist score significantly improved
- Grip was unaffected, whereas pinch (the ability to pinch) improved at six-month follow-up)
A December 2022 paper (12) compared the effects of repeated cortisone injections at 3 months and beyond in patients treated for knee osteoarthritis or trapeziometacarpal osteoarthritis to patients receiving hyaluronic acid, platelet-rich plasma, or placebo. The study found the hyaluronic acid, platelet-rich plasma, and placebo injections to be superior treatments 24 months after the injection.
Conclusion: “PRP injection for symptomatic trapeziometacarpal osteoarthritis is a reasonable therapeutic option in early stages.”
A January 2023 study (13) assessed the effectiveness of platelet-rich plasma (PRP) injection among patients with thumb carpometacarpal (CMC) joint osteoarthritis. In this study nineteen adult patients (9 women; average age 65) who received a PRP injection for osteoarthritis in one or both thumb carpometacarpal (CMC) joints were studied. The results: “Subjects reported moderate or excellent symptom improvement in 68.8% of injected joints and were moderately or very satisfied with 68.8% of the procedures. Mean patient-reported duration of benefit was 15.6 months . . .”
Autologous fat injections and Platelet-Rich Plasma injections
A January 2023 review study (14) compared autologous fat injections and Platelet-Rich Plasma injections for Trapeziometacarpal Osteoarthritis. Autologous fat injections are given to help patch cartilage deficits. The authors of the study write: “(Injection) therapy with autologous substances such as platelet-rich plasma and autologous fat have recently gained increasing attention because of beneficial pain-reducing effects in arthritis and the associated regenerative potential.” In this review study, the researchers found both autologous fat injections and Platelet-Rich Plasma injections “achieved a good and long-lasting pain reduction, which may also be accompanied by corresponding improvement in hand function.”
Doctors at the University of Malaga in Spain presented this case study of a concert pianist helped by PRP
This case review (15) was published in October 2019:
“Thumb carpometacarpal osteoarthritis is a progressively disabling, debilitating condition presenting with thumb base pain and hand functional impairment. Platelet-rich plasma has been used widely for the management of musculoskeletal pathologies, osteoarthritis being among them.
- A 59-year-old male professional pianist presented with chronic, mild onset of right thumb base pain involving a progressive lack of pinch strength in his right hand, and severe difficulties with playing.
- Three PRP injections were administered to the Thumb carpometacarpal joint on a 1-week interval regime.
- Clinical outcomes were assessed by using standard scoring scales including those for pain, grip and pinch strength
- Functional outcome was excellent according to patient’s capability with daily living activities and specific playing demands.
- At 12 months follow-up, no recurrences or complications were identified, with the musician returning to his previous level of performance 2 weeks before the end of this period.
“Patient self-reported satisfaction was high and he reported to return to his routine piano activity with no limitations. This case-based review study documents the clinical efficacy of PRP treatment from both functional and perceived-pain perspectives in a professional pianist. Presenting this case, our aim is to draw attention of healthcare providers dealing with Thumb carpometacarpal osteoarthritis to PRP as a safe, beneficial therapy for this condition which needs further assessment in randomized controlled trials.”
Bone marrow derived stem cell therapy for thumb osteoarthritis
There is research coming suggesting that the positive effects of stem cell therapy studied and documented in the large joints, the hips and knees for example, can be demonstrated in the small joints, those of the thumb for example. This was suggested and shown by research in the journal Plastic and reconstructive surgery. Global open. (16)
Independent research: “Many patients showed improved quality of life and pain relief. These injections appear to be an effective means of postponing surgery”
A November 2021 study (17) evaluated the effect of bone marrow aspirate concentrate (BMAC) in the treatment of osteoarthritis of the thumb first carpometacarpal joint. Injections were carried out in 27 thumbs.
According to the Dell classification (a scoring system to determine the severity of the thumb osteoarthritis from Stage I less joint space narrowing to Stage IV severe osteoarthritis), there were:
- 2 stage I,
- 11 stage II,
- 13 stage III
- and 1 stage IV cases examined.
The bone marrow was aspirated from the iliac crest, concentrated by centrifugation, and injected under fluoroscopic control into the pathological thumb. Results were assessed at a average 16 months’ follow-up.
Clinical evaluation comprised of:
- QuickDASH (A disability scoring system that ranges from – 0 (no disability) to 100 (complete disability) and PRWE (Patient-Rated Wrist Evaluation – A disability scoring system for the wrist that ranges from – 0 (no disability) to 100 (complete disability) scores, pain at rest on a numerical analog scale (NAS a zero – 10 (worst) scoring system), and thumb column abduction.
- QuickDASH and PRWE scores were 59 (range, 27-82) and 88 range, 37-125) preoperatively and 29 (range, 0-64) and 50 (range, 1-99) postoperatively, respectively.
- Mean pain at rest on NAS improved from 7 (range, 1-10) to 4 (range, 0-9).
- Thumb abduction improved by a mean 18° over preoperative data.
- No postoperative complications were found.
- Two patients had to be operated on for inefficacy of injection.
The researchers noted: “This is the first article presenting the effect of an intra-articular injection of bone marrow aspirate concentrate in the thumb first carpometacarpal joint and the results were encouraging. Many patients showed improved quality of life and pain relief. These injections appear to be an effective means of postponing surgery.”
Research summary
PRP and stem cell therapy can help many people. A 2021 paper (18) offers us a summary of the research:
“The intra-articular injection of therapeutic agents is an attractive strategy for the local treatment of Thumb-Base Osteoarthritis. . . However, the current evidence remains equivocal. The main reason behind this is related to the poor methodology of the available scientific studies, which makes the results quite inconclusive. Some data supported the clinical usefulness of intra-articular hyaluronic acid, especially in improving functional capacity and of intra-articular corticosteroids in reducing painful symptomatology; new emerging and encouraging results derived from PRP and mesenchymal-derived stem cell populations, but they are still preliminary. At this regard, we auspicate a growing development of the scientific evidence in the field of regenerative medicine until now poorly explored in Thumb-Base Osteoarthritis. “
Treating the whole body when treating the thumb
We will often see patients who have many joints that hurt and seek help in treating multiple joints at a time. Research has shown that treating one joint without addressing the others could lead to less than successful patient outcomes whether with conservative care treatments or surgical treatments. An August 2023 paper (19) looked at how often patients with thumb osteoarthritis has osteoarthritis in other joints and did problems in the other joint affect their thumbs negatively. In this study of 145 patients with an average age of 62 years and 72% were female, researchers found an average of 3.6 other joints hurt. Of the patients, 10% reported only their hands as being symptomatic; 30% reported 2-3 other symptomatic sites, and 49% reported 4 other joints hurt them. The researchers found that the more joints that hurt, the weaker the grip strength and less favorable reported outcomes from conservative or surgical care.
Call for a free phone consultation with our staff 800-300-9300
References:
2 Warwick D, Fetouh S. Diagnosis and Treatment of Carpometacarpal Instability. Hand Clinics. 2022 May 1;38(2):261-8.
6 Brandt KD, Radin P, Dieppe P, Putte L. Yet more evidence that osteoarthritis is not a cartilage disease. Ann Rheum Dis. 2006;65(10):1261-1264.
7 Mosegaard SB, Stilling M, Hansen TB. Risk factors for limited improvement after total trapeziometacarpal joint arthroplasty. Health and Quality of Life Outcomes. 2020 Dec;18:1-8.
8 Gay AM, Cerlier A, Iniesta A, Legré R. Surgery for trapeziometacarpal osteoarthritis. Hand Surgery and Rehabilitation. 2016 Sep 30;35(4):238-49.
9 Knightly N, Sullivan P. Surgery for Trapeziometacarpal Joint Osteoarthritis: A Meta-Analysis on Efficacy and Safety. The Journal of Hand Surgery Asian-pacific Volume. 2021 Jun 1;26(2):245-64.
10 Malahias MA, Roumeliotis L, Nikolaou VS, Chronopoulos E, Sourlas I, Babis GC. Platelet-Rich Plasma versus Corticosteroid Intra-Articular Injections for the Treatment of Trapeziometacarpal Arthritis: A Prospective Randomized Controlled Clinical Trial. Cartilage. 2018 Oct 20:1947603518805230.
11 Loibl M, Lang S, Dendl LM, Nerlich M, Angele P, Gehmert S, Huber M. Leukocyte-reduced platelet-rich plasma treatment of basal thumb arthritis: a pilot study. BioMed Research International. 2016 Jul 5;2016.
12 Donovan RL, Edwards TA, Judge A, Blom AW, Kunutsor SK, Whitehouse MR. Effects of recurrent intra-articular corticosteroid injections for osteoarthritis at three months and beyond: a systematic review and meta-analysis in comparison to other injectables. Osteoarthritis and Cartilage. 2022 Sep 13.
13 Hasley IB, Bies MM, Hollman JH, Carta KG, Sellon JL, Brault JS. Platelet-Rich Plasma Injection for Thumb Carpometacarpal Joint Osteoarthritis. Archives of Rehabilitation Research and Clinical Translation. 2023 Mar 1;5(1):100257.
14 Winter R, Hasiba-Pappas SK, Tuca AC, Zrim R, Nischwitz S, Popp D, Lumenta DB, Girsch W, Kamolz LP. The effect of autologous fat grafting and platelet-rich plasma injections in osteoarthritis of the CMC joint of the thumb: a systematic review and meta-analysis. Plastic and Reconstructive Surgery. 2022 Oct 11:10-97.
15 Medina-Porqueres I, Martin-Garcia P, Sanz-De Diego S, Reyes-Eldblom M, Cantero-Tellez R. Platelet-rich plasma for thumb carpometacarpal joint osteoarthritis in a professional pianist: case-based review. Rheumatology international. 2019 Oct 14:1-9.
16 Murphy MP, Buckley C, Sugrue C, Carr E, O’Reilly A, O’Neill S, Carroll SM. ASCOT: Autologous Bone Marrow Stem Cell Use for Osteoarthritis of the Thumb-First Carpometacarpal Joint. Plast Reconstr Surg Glob Open. 2017 Sep 19;5(9):e1486. doi: 10.1097/GOX.0000000000001486. PubMed PMID: 29062653; PubMed Central PMCID: PMC5640358.—
17 Daoudi I, Pélissier P, Dargai F, Choughri H, Delgove A. Intra-articular injection of autologous bone marrow aspirate concentrate in the treatment of osteoarthritis of the thumb first carpometacarpal joint: A pilot study. Hand Surgery and Rehabilitation. 2021 Nov 11.
18 Tenti S, Cheleschi S, Mondanelli N, Giannotti S, Fioravanti A. New Trends in Injection-Based Therapy for Thumb-Base Osteoarthritis: Where Are We and where Are We Going?. Frontiers in Pharmacology. 2021 Apr 13;12:498.
19 Perruccio AV, Badley EM, Power JD, Baltzer H. Frequency of multisite non-hand joint involvement in patients with thumb-base osteoarthritis, and associations with functional and patient-reported outcomes. Osteoarthritis and Cartilage Open. 2023 Aug 10:100397.
20 Tveter AT, Østerås N, Nossum R, Eide REM, Klokkeide Å, Matre KH, Olsen M, Kjeken I. Long-term changes in pain and function in patients with thumb base osteoarthritis receiving brief information, occupational therapy and/or surgery. Musculoskeletal Care. 2024 Jun;22(2):e1883. doi: 10.1002/msc.1883. PMID: 38629865. *






