Chronic neck pain is one of the more frequent problems we see in our new patients because of its complexity and difficulty in finding the true cause of pain.
Patients may present themselves with numbness or pain radiating from the neck into the arm due to nerve compression. They may be diagnosed with cervical radiculopathy which is caused by herniated disc, or spondyliotic foraminal stenosis. When many doctors think there is a radiculopathy, a surgery will be recommended.
Watch Dr. Grove discuss various issues of the neck
Part 1
Part 2
Chronic neck pain usually centers around the nerves.
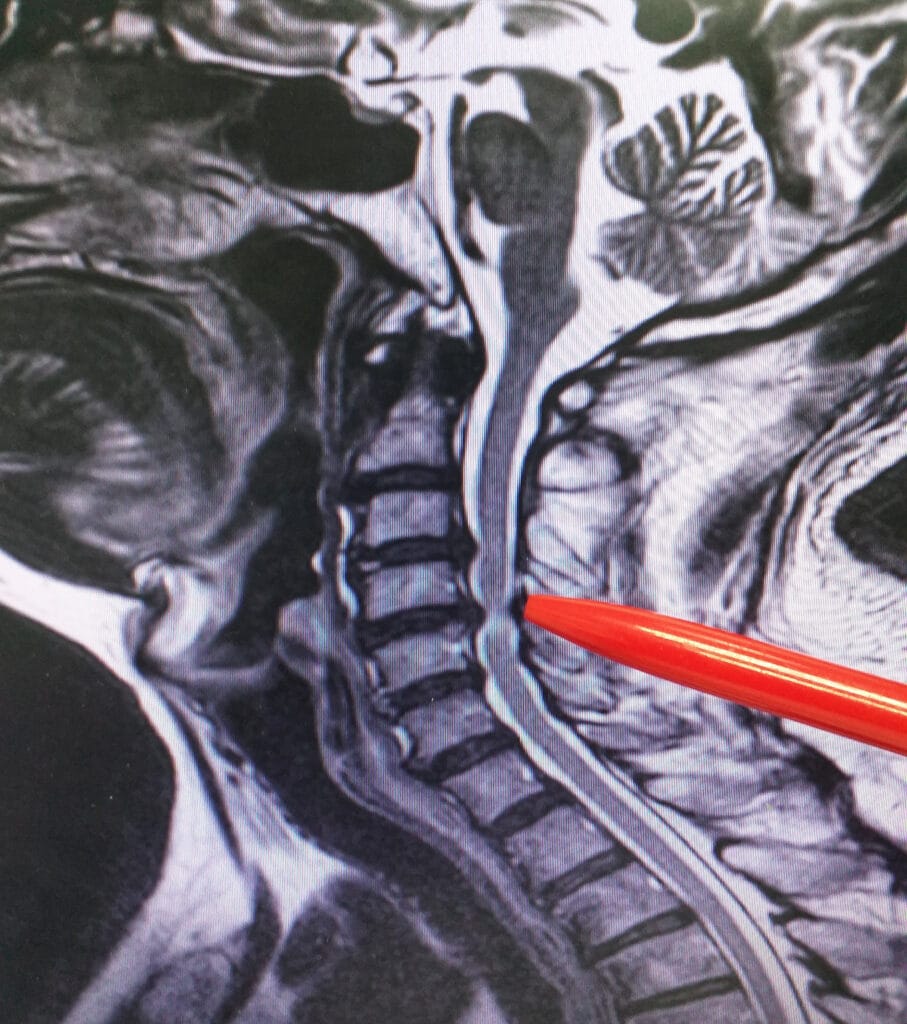
Chronic neck pain usually centers around the nerves. A disc in the neck can become herniated or “bulge” because of the wear and tear of the tendons, ligaments, and muscles. One possible diagnosis out of many may be spondylolisthesis – where one vertebra slides forward over the bone below it. Another reason neck pain is so prevalent is that the weight of the head is not proportionate to the strength and size of the neck, you do not have a good ability to hold your head up.
Sometimes in an attempt to stabilize the weakened area of the neck, bone spurs will form (osteoarthritis) to “hold things in place.” It is at this point “conservative treatments” for alleviating the pain of the neck area are used. This can begin with a steady diet of anti-inflammatory medications to ease the nerve pain. Cortisone may be injected to reduce inflammation and swelling.
Chiropractics is often tried to push the vertebrae back into place and usually it does, but the vertebrae will slip back because of loose ligaments that chiropractors can cause, and the pain cycle starts again. As pain increases, the surgical consultation is considered. To prevent pain, either bone is chipped away from the nerves (laminectomy) or a cervical fusion to prevent the vertebrae from slipping out of place is recommended. Fusion surgery is of course a complicated surgery, metal and/or bone is attached to the vertebrae and “fused” together to prevent the vertebrae from moving and cause distress on the nerves. Fusion surgery has its draw backs. First, even if successful, the fusion will limit the patient’s mobility in the neck region.
Second, the fusion can cause a “different pain,” because new stress is placed on the non-fused area above and below the fusion. Third, new pain can be caused by the damage of the surgery to connective and supportive tissue, i.e., ligaments and tendons already in a weakened state.
Neck specific exercises and physiotherapy
A January 2023 study (1) found that both neck specific exercises and Physiotherapy could significantly help patients with headaches and dizziness as a result of cervical radiculopathy. The exercises started with isolated low-load sensorimotor exercises and progressed to endurance exercises. “The individual physical activity consisted of a recommendation of an aerobic and/or muscular physical activity or training, and the general prescription consisted of at least 30 minutes of physical activity at moderate intensity three times per week.” Discuss with your health care provider which exercises would benefit you the most.
Treating cervical ligaments to restore neck stability
In our office, treating chronic neck pain begins with the repair and strengthening of cervical ligaments. Ligaments are the connective tissue that hold your cervical spine vertebrae in place and your neck in its correct anatomical alignment. When your ligaments are weak, they can no longer hold the neck in proper alignment. When the neck is not in alignment the vertebrae can pinch nerves, constrict arteries, put pressure on your esophagus among other problems that may cause the myriad of symptoms people relay to us in their emails.
C1-C2 instability and a reverse curve
Of the many emails that I get are ones which discuss C1-C2 cervical spine instability. Many emails will talk about chronic upper cervical subluxation at C1-C2 and a reverse curve. The normal curve of the spine is shaped like a backwards “C.” If you have a problem with your neck, Lordosis is probably a word you are very familiar with. When your curve went from a natural “C” shape to a reverse curve you were probably told you had a reversed lordosis or your neck had become Kyphotic. Your neck is now curving in the opposite direction. This may be causing a lot of pain. Some of the pain maybe from muscle spasms. As the muscles are trying to stabilize the spine, the extra workload causes spasms.
When the spine is moving towards a reversed curve, adjacent segments may show cervical disc degeneration at lower levels such as C2-C3, C3-C4. These are the problems which will lead many people to a cervical spine fusion.
Injection treatments
An October 2021 paper (2) suggests that “Evidence is growing to support the use of regenerative injection treatments, including prolotherapy, platelet-rich plasma (PRP), platelet lysate (PL), and mesenchymal stromal cells. . . PRP is a safe injectate that shows promise for effective treatment of axial neck pain when utilized in a thoughtful manner targeting ligamentous laxity, intraarticular facet arthritis, and nerve root irritation. Though this early data is encouraging, more comprehensive, randomized controlled trials including a larger number of patients are needed to further validate these findings. Given the significant impact of neck pain on quality of life for an aging population, an overreliance on opioid medications for the management of chronic musculoskeletal pain by providers, and the significant societal costs, both directly and indirectly, a more comprehensive treatment approach from a biomechanical perspective that offers the possibility of disease modification rather than symptom management is needed.”
Comparing regenerative injections, decompression and pain-killer and anti-inflammatory approaches to cervical radiculopathy.
A December 2020 study (3) analyzed the equivocal evidence in support of the effectiveness of each of the three co-existing approaches to conservative treatment of cervical radiculopathy: biological (regenerative), mechanical (decompression) and physical (analgesic and anti-inflammatory). These treatments were compared by dividing 90 patients into six treatment groups.
- Biological treatment: 4 ultra-sound-guided periradicular injections of ACS (Autologous conditioned serum) or PRP (1 per week);
- Mechanical treatment: manual therapy or traction therapy – 8 sessions (two per week);
- Physical treatment: laser therapy or collagen magnetophoresis (the use of a magnetic field in collagen application) – 8 sessions (two per week).
Comparison findings:
- Biological treatments were more effective than mechanical and physical therapies in reducing pain, improving the disability index and proprioception of the hand both immediately on completion of therapy and after a follow-up period, which may suggest their regenerative properties.
- Physical and mechanical therapies produced improvement in the above-mentioned indicators on completion of the therapy, but subsequently exerted a very slight effect during the follow-up period without evident regenerative effects; moreover, a regression of the results was actually recorded for traction therapy. Caution should be paid when using traction therapy in the acute period of root edema, due to possible signs of intolerance of the procedure and exacerbation of the discomfort.
A March 2023 review study however (4) looked at 10,514 studies to see if a comparison could be made between traditional conservative care treatments versus surgical treatment for cervical radiculopathy. Forty-two studies provided baseline motor radiculopathy data, only 22 provided follow-up motor outcomes. The largest group of patient data the researchers had was the group that had surgically-managed motor radiculopathy with unclear pain status. There were no group measurements found for “conservatively-managed painless motor radiculopathy”. The researchers noted: “Large disparities in data quality made direct comparison of conservative vs operative management difficult. . . Many studies fail to report motor outcomes after intervention, meaning statistical evidence to guide optimal management of motor radiculopathy is currently lacking. ”
Restoring cervical neck stability by repairing and regenerating the neck ligaments
Many patients with these problems will talk about dizziness or even Bell’s Palsy. They also talk about 2 – 3 times a week chiropractic adjustments. When the patient says they are having success at the chiropractor with their cervical lordosis and their symptoms of dizziness, we know that we can have a realistic expectation that we can help. The chiropractic is helping because the vertebrae are pushed back towards a natural alignment. The reasons that the patient needs to see the chiropractor 2 – 3 times a week is because the the adjustments are not holding. We do get many referrals from chiropractors to help their patients by strengthening the cervical ligaments with our injection treatments.
Platelet Rich Plasma injections
PRP treatments involve collecting a small amount of your blood and spinning it in a centrifuge to separate the platelets from the red cells. The collected platelets are then injected back into the injured area to stimulate healing and regeneration. Research has shown PRP can be effective in treating degenerative disc disease by addressing the problems of cervical spine ligament instability. The treatment will not work for everyone.
Stem cell injections
Stem cell injections involve the use of Bone Marrow derived stem cells. The injections help restore ligaments strength by causing the regeneration of ligament, tendon, cartilage and bone regeneration. The treatment will not work for everyone.
Call for a free phone consultation with our staff 800-300-9300
References
1 Svensson J, Peolsson A, Hermansen A, Cross JJ, Abbott A, Cleland JA, Kierkegaard M, Halvorsen M, Dedering Å. The effect of neck-specific exercise and prescribed physical activity on headache and dizziness in individuals with cervical radiculopathy: Further analyses of a randomized study with a 1-year follow-up. Physiotherapy Theory and Practice. 2024 Apr 2;40(4):714-26.
2 Godek P, Murawski P, Ruciński W, Guzek M. Biological, Mechanical or Physical? Conservative Treatment of Cervical Radiculopathy. Ortopedia, Traumatologia, Rehabilitacja. 2020 Dec 1;22(6):409-19.
3 Williams C, Jerome M, Fausel C, Dodson E, Stemper I, Centeno C. Regenerative Injection Treatments Utilizing Platelet Products and Prolotherapy for Cervical Spine Pain: A Functional Spinal Unit Approach. Cureus. 2021 Oct 8;13(10).
4 Gebreyohanes A, Erotocritou M, Choi D. Appraising The evidence for conservative versus surgical management of motor deficits in degenerative cervical radiculopathy. Global Spine Journal. 2023 Mar;13(2):547-62.






