The hip joint, the shoulder joint, the knee joint, the big toe joints, they all have one thing in common. When they are in the process of wear and tear degenerative joint disease, they become unstable, painful, and they start forming bone spurs and bony overgrowths. Sometimes the person suffering from degenerative joint disease will let this condition of joint instability go on for too long. This will cause the bone spurs to become too large and they will freeze up the joint, making it stiff and unmovable, and, necessitating a need for surgery to shave down the bones. In the big toe, this bone spur or overgrowth is commonly referred to as a bunion.
In this article I will discuss with you the two main type of patients we see with big toe pain. The patient who has big toe joint instability that can be helped with certain injections and the patient with a large bunion and what we may be able to do for them.
The big toe has two joints
- metatarsophalangeal joint (the bunion joint)
- interphalangeal joint (the joint under the toenail)
The metatarsophalangeal joint is where we will concentrate this article.
The reality of non-surgical options for hallux valgus or more commonly a “bunion.”
In June 2022 (1) researchers began a study to explore the use of non-surgical treatments for hallux valgus. The authors write: “Non-surgical management of hallux valgus may involve footwear advice or modification, foot orthoses, night splints, and physical therapies (manual therapy, taping or foot exercises). In podiatric clinical practice, these interventions are often combined in a multifaceted approach. However, there is limited evidence for the effectiveness of any of these interventions. . . . The available evidence provides preliminary support for the use of footwear, foot orthoses and foot exercises for the treatment of hallux valgus, but these three promising approaches are yet to be evaluated in combination.”
Then in a November 2023 paper, (2) researchers demonstrated that it is difficult to test whether non-surgical options are viable for bunions and foot deformities. They write: “In its current form, a randomized trial of footwear, foot orthoses, foot exercises, advice and self-management for relieving pain associated with hallux valgus is not feasible, particularly due to the low adherence with the intervention.” One problem is that the study participants did not think these interventions worked.
We are often asked about helping “turf toe” or the accompanying inflammation sesamoiditis, the inflammation at the base of the big toe. Many of the people who do reach out to us about their toes report that not only do they have pain and inflammation in their toe, but these problems are also causing significant problems in bending their toe at the base when they walk.
By the time they reach out to us they have tried to manage their toe pain on their own with anti-inflammatories, toe tape, toe sleeves, shoe inserts and hard splints among many other remedies. One the pain and function is too much for them to handle on their own, that is when they started making doctor appointments. At the first doctor appointment they were told to “stay off it,” rest, and take more anti-inflammatories. If the problem persisted, there was a chance that they had a cortisone injection, a better shoe insert, a walking boot, even physical therapy. If this did not work, there would be a discussion about surgery.
A 2020 study in the journal Foot and ankle surgery (1) sought to expand the understanding of big toe instability or “turf toe,” as “a wide variety of traumatic lesions of the first metatarsophalangeal joint).” “Turf toe,” refers to injuries typically sustained by athletes who play on turf. These are lesions (tears and damage) are typically difficult to diagnose, with a large variation of outcomes and a potential to impair patients’ functional performance on a definitive and perennial basis.” In other words, big toe pain can be caused by many things and cause a lot of problems. Treatment has been challenging because doctors have focused on a limited aspect of the big toe pain – the metatarsophalangeal joint and not the understanding of the whole foot dynamic.
The researchers of this study used their “Expanded Turf-toe” diagnosis, incorporating various injuries originally thought to be outside the traditional diagnosis of “Turf toe.” This would include injuries to someone, maybe like yourself, who is not athletic but suffers from the same type of toe pain and instability.
- The most frequent cause of injury was axial load with various direction of stress at the first MTP. (This would be a position where your toes would be flat on the ground and your heel would be several inches off the ground. A position achieved by the wearing of high heeled shoes or toe raising exercise.)
This injury caused these problems typical of whole joint instability:
- hallux varism (the anatomical distorting of the big toe) in 42% of the study subjects
- pure hyperextension (the toe is exceeding is normal range of motion) in 42% of the study subjects,
- extension with hallux valgism (The beginnings of the formation of a bunion to stop the abnormal range of motion from causing more damage in 21% of the study subjects),
- pure hyperflexion (the muscles of the toe are now extending beyond their normal range of motion) in 8% of the study subjects,
- and hyperflexion with hallux valgism (the muscles of the toe are now extending beyond their normal range of motion with bunion formation starting) in 4% of the study subjects,
With all this instability and hypermobility it is easy to understand your toes’ desire to start forming bone spurs to keep itself together.
Caring for big toe joint instability
PRP treatments involve collecting a small amount of your blood and spinning it in a centrifuge to separate the platelets from the red cells. The collected platelets are then injected into toe joints to stimulate healing and regeneration.
Doctors an researchers also suggest bone marrow derived stem cells may help some patients. These cells are also injected into the joint to stimulate healing and regeneration. The decision on what treatment path to follow is made during the initial consultation and physical examination of the toe.
The goal of regenerative therapy is to stabilize the big toe and prevent the formation of a bunion.
- Regenerative medicine seeks to repair loose and damaged ligaments which have allowed the bones of the toe to move in abnormal ways and led to the grinding and crunching that destroys the joint’s cartilage.
- Regenerative medicine focuses on the tendon attachments to the bones. This damage allows the muscles of the toe to hyperflex, injuring both the muscle and allowing the joint the abnormal motion that damages the cartilage.
A December 2018 study (2) evaluated clinical improvement in a population of elite dancers following treatment with ultrasound-guided platelet-rich plasma (PRP) injections of various lower extremity sites by assessing when they were able to return to dance.
- Nineteen dancers (13 female, 6 male; ages 15 to 42) were treated between 2009 and 2016 at sites that included: hamstring tendon (1), proximal iliotibial band (1), patellar tendon (3), posterior tibial tendon (5), peroneus brevis tendon (3), plantar fascia (3), and the first metatarsophalangeal (MTP) joint capsule (3).
- All patients adhered to standard post-care instructions, including non-weightbearing and avoidance of NSAIDs for at least 2 weeks post-injection.
- Eighteen subjects achieved return to dance, 13 in 6 months or less, and the majority (10) within 3 months of injection. Five subjects required more than 6 months recovery time. These cases all involved foot and ankle sites; of these, two subjects required repeat injections, and both returned to dance within 11 months of the second injection
It should be pointed out that we carry out a more aggressive protocol for dancers and athletes that need to return to activity as quickly as possible.
Minimally invasive surgery for severe hallux valgus
A June 2022 study (5) examined minimally invasive surgery for severe hallux valgus in 106 feet. The researchers write: “There is widespread variation in the optimal procedure for correction of severe hallux valgus deformity . . . This study has demonstrated third-generation minimally invasive chevron and Akin osteotomies (MICA) for the treatment of severe hallux valgus deformity enables substantial deformity correction and is associated with significant improvements in clinical patient reported outcomes two years following surgery.
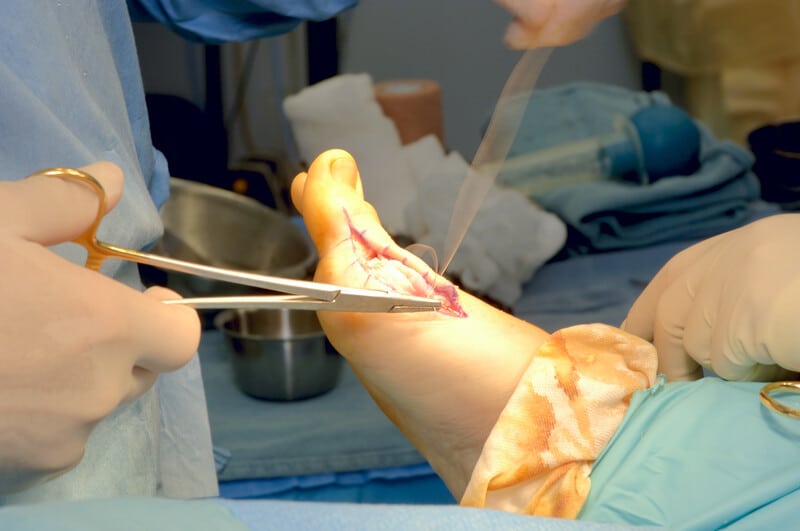
Is Bunion shaving necessary?
Bunion shaving is not always the answer. Shaving down the bunion will provide some people with immediate relief and a more natural looking toe. However, research in showing us that shaving down the bunions is far from the end of the story. This is from a recent study in the journal Clinical biomechanics.(3) Here researchers wrote: “. . . our study showed that the hallux valgus deformity is not only a problem of the foot’s structure and function but also affects the entire lower limb and even the pelvis motion during walking. Surgical correction of the deformed segment (the bunion) itself could only correct skeletal alignment. However, (shaving the bunion down) does not solve functional related problems that occur during walking that are probably related with the cause of the problem . . . ” Simply, shaving the bunion down does not correct the problem of what caused the bunion to form in the first place. If the instability in the toe and foot are not corrected, the bunion will form again.
In the patient who has significant bunion formation, bunion removal may be needed. For others, correcting the problem of toe and foot instability may provide enough treatment to correct the alignment of the toe and eliminate the need for surgery. The recommendation for or against surgery is always best made after an examination.
Stem Cell Therapy for cartilage repair
There is not much research on stem cell therapy for big toe arthritis pain. There is a lot of research on osteoarthritis. You can find this research in my article on stem cell therapy. Many doctors have noted empirically that stem cell therapy helps many people with toe pain. Stem cells are “de-differentiated pluripotent” cells, which means that they continue to divide to create more stem cells; these eventually “morph” into the tissue needing repair — collagen, bone, and cartilage.
References:
1 Nery C, Fonseca LF, Gonçalves JP, Mansur N, Lemos A, Maringolo L. First MTP joint instability—Expanding the concept of “Turf-toe” injuries. Foot and Ankle Surgery. 2018 Nov 22.
2 Jain N, Bauman PA, Hamilton WG, Merkle A, Adler RS. Can Elite Dancers Return to Dance After Ultrasound-Guided Platelet-Rich Plasma (PRP) Injections?. J Dance Med Sci. 2018;22(4):225‐232. doi:10.12678/1089-313X.22.4.225
3 Klugarova J, Janura M, Svoboda Z, Sos Z, Stergiou N, Klugar M. Hallux valgus surgery affects kinematic parameters during gait. Clin Biomech (Bristol, Avon). 2016 Dec;40:20-26. doi: 10.1016/j.clinbiomech.2016.10.004. Epub 2016 Oct 6. PubMed PMID: 27792950; PubMed Central PMCID: PMC5325701.
4 Menz HB, Lim PQ, Hurn SE, Mickle KJ, Buldt AK, Cotchett MP, Roddy E, Wluka AE, Erbas B, Munteanu SE. Footwear, foot orthoses and strengthening exercises for the non-surgical management of hallux valgus: protocol for a randomised pilot and feasibility trial. Journal of Foot and Ankle Research. 2022 Dec;15(1):1-0.
5 Lewis TL, Ray R, Gordon DJ. Minimally invasive surgery for severe hallux valgus in 106 feet. Foot and Ankle Surgery. 2022 Jan 31.






