Marc Darrow, MD, JD
In this article I will address recent research published by the surgical community on knee replacement complications. Most people have very good outcomes with knee replacements. Many people continue to have lingering problems following their knee replacement. Most of the problems come from mechanical and hardware problems and are often addressed in a revision surgery. Many complain of their inability to bend their knees, continued pain, stiffness and rigidity, knee instability when walking. Many of these problems can be addressed with physical therapy and strengthening of the surviving ligaments, tendons and muscle attachments, as in regenerative medicine injections.
What I will review in this article:
- Revision knee replacement surgery may not fix the knee replacement problems.
- Knee replacement survival rate in younger and middle-aged patients may lead to a second knee replacement in the future.
- Pre-surgery depression an anxiety may impact knee replacement outcomes.
- “It doesn’t feel like my knee”: Sensations of discomfort, including heaviness, numbness, pressure, and tightness associated with the prosthesis.
- Do Women Have More Knee Replacement Complications?
- How fast can you get back to work or sport following knee replacement?
Listen to the noise coming from this knee replacement
Revision surgery does not fix the knee replacement to levels of successful primary knee replacement
A February 2024 study (1) reviewed patient reported outcomes following a revision knee replacement surgery. They found that patients who underwent revision total knee replacement (all causes) had lower rates of improvement and higher rates of worsening compared to patients who had only a primary total knee replacement. This suggests that patients who had failed primary knee replacement, the revision surgery will not make outcomes as good as a successful primary knee replacement. The patients of this study reported that physical function specifically a problem. The researchers here also noted that. “Although primary total knee replacement patients did better overall, the improvement rates may be considered relatively low and should prompt discussions on improving outcomes following primary total knee replacement and revision total knee replacement.”
Knee replacement survival rate in middle-aged patients up to 65 years old
An April 2023 paper in the journal Cartilage (2) documented the knee replacement survival rate in middle-aged patients up to 65 years old and to compare it with other age groups of patients undergoing total knee replacement for knee osteoarthritis. Over 45,000 patients were in this study.
Learning points:
- A total of 45,488 total knee replacement patients for primary knee osteoarthritis were included in the analysis. Of this there were 11,388 men and over twice as many women: The number of women was 27,846).
- The percentage of knee replacement patients less than 65 years old increased from 13.5% to 24.8% between 2000 and 2019. (Many more knee replacements (increases) in this group.)
- The survival analysis showed an overall influence of age on the implant revision rate.
- Patients under 50 years old estimated survival rate of 78.7% at 15 years (revision knee surgery or other procedure will need to be done at age 65 for over 20% of patients)
- Patients 50-65 years estimated survival rate of 89.4% at 15 years (revision knee surgery or other procedure will need to be done at age 65 to age 80 for over 10% of patients)
- Patients 66-79 years estimated survival rate of 94.8% at 15 years.
Conclusions: “Total knee replacement us in the middle-aged patient population up to 65 years old increased significantly over time. These patients present a double risk of failure with respect to older patients. This is particularly important considering the increasing life expectancy and the emergence of new joint preserving strategies (including knee injections), which could postpone the need for total knee replacement to an older age.
Depression, anxiety and negative attitude may impact knee replacement outcomes
It doesn’t feel like my knee: Sensations of discomfort, including heaviness, numbness, pressure, and tightness associated with the prosthesis
While knee replacement can sometimes be a viable and effective treatment for patients with knee osteoarthritis, the number of patients asking about knee replacement alternatives continues to grow. Patients need to be aware of the potential downsides of the procedure, particularly in light of the new therapies available.
Over the years I have seen many patients who still had knee pain following knee replacement surgery. What I see in my practice agrees with what medical research states—that knee replacement surgery offers hope to some patients, and these patients have high expectations of what the new knee will offer them, but that in many cases those expectations are not met.
English doctors wrote in a June 2022 study (7) that up to 20% of people who undergo total knee replacement surgery have ongoing pain and discomfort. The researchers write:
- Patients describing chronic postsurgical pain also “described sensations of discomfort, including heaviness, numbness, pressure, and tightness associated with the prosthesis.
- Participants reported “a lack of felt connection with and agency over their replaced knee, often describing it as alien or other, and lacked confidence in the knee.”
“patient-perceived enlargement of knee.”
A June 2022 paper (8) suggests that in clinical practice, many patients complained that their knees became larger after total knee arthroplasty, yet no studies have described this phenomenon. The study authors then named this as “patient-perceived enlargement of knee.”
In this study the researchers reviewed patients that underwent unilateral primary total knee arthroplasty between May 2018 and April 2019. They investigated the prevalence of “patient-perceived enlargement of knee” and acquired functional scores and satisfaction. Patients were divided into two groups according to whether they complained of “patient-perceived enlargement of knee.”
A total of 389 patients were enrolled and 101 patients felt their knee became “larger” after total knee arthroplasty. Patients with patient-perceived enlargement of knee had significantly shorter height and lower weight, yet component size distribution showed no statistical difference. Patients with patient-perceived enlargement of knee had significantly lower functional scores and satisfaction.
Anterior femoral notching and fractures after total knee replacement.
During total knee replacement surgery, the thigh bone can get cut in the front inadvertently. This is called Anterior femoral notching. A July 2022 paper (9) noted that anterior femoral notching (AFN) is a severe complication of total knee replacement, which in a percentage of patients may lead to fractures after surgery. What the researchers noticed in patients with Anterior femoral notching is that during their gait cycle, if there is an anterior femoral cortical notch more than 3 mm, the stress will be significantly increased and that maximum equivalent stress exceeded the femoral yield strength and may increase the risk of periprosthetic fractures.
Does having bowlegged knee osteoarthritis or knock knee osteoarthritis make a difference in treatments?
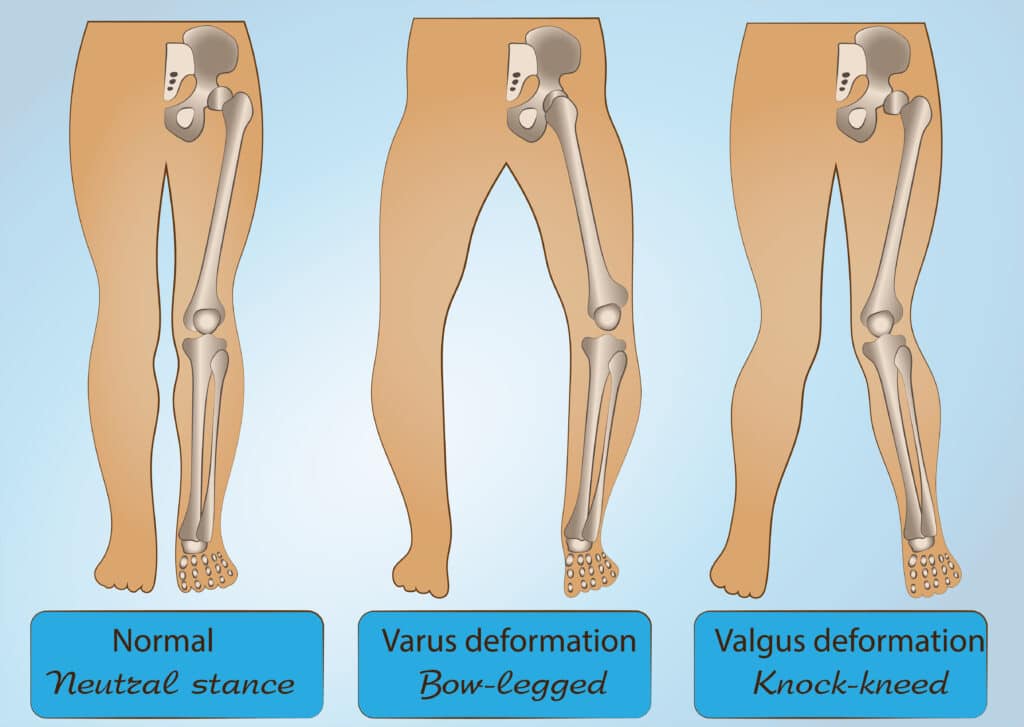
In an April 2023 study (10), doctors examined the medical histories of 834 people to see if people with bowlegged knee osteoarthritis or knock knee knee osteoarthritis patients could avoid knee replacement surgery with conservative care treatments. The researchers looked at patients with advanced knee osteoarthritis, Kellgren-Lawrence knee osteoarthritis grades III and IV. These patients were divided into varus arthritic bow-legged knee (bow-legged) or valgus arthritic knee, knock-knees. They found that the valgus arthritic knees responded better to conservative treatment than varus arthritic knees and had less chance of needing knee replacement. Five years after the start of conservative care treatments 76.8% of varus – bow legged patients needed knee replacement while 38.6% of valgus arthritic knee patients went on to knee replacement.
In this image, the man has varus arthritic knees, more commonly known as being “bow-legged.” Bow legged people are at higher risk for needing knee replacement.
One of the challenges of knee replacement is under correction of valgus deformity
A March 2023 (11) investigated the effect of different degrees of valgus deformity correction on patellar position and clinical outcome in 118 patients with valgus knees after total knee replacement minor valgus under correction did not affect the short-term outcome after total knee replacement; however, when the residual valgus angle was greater than 6°, the post-operative scores were significantly reduced. The researchers also noted: “Inadequate valgus correction does not result in significant changes in patellar height but may increase the risk of poor patellar tracking.”
Pes anserinus pain syndrome
A June 2020 paper (17) looked at pes anserinus pain syndrome as a cause of post-knee replacement pain. In 389 primary total knee replacements patients, researchers found 5.6% (22/389 patients had pes anserinus pain syndrome). Higher risk factors were:
- female
- overweight / obese
Those suffering with pes anserinus pain syndrome were treated non-operatively; 81.8% responded to nonsteroidal anti-inflammatory drug-physical therapy program and 18.2% required an additional local steroid injection.
More hospital readmissions
The researchers of this study concluded that “rehabilitation (following surgery) must focus not only on strengthening the joint and promoting full recovery to tasks but on modifying a person’s relationship to the new joint and managing sensations of otherness to achieve full incorporation of the joint or re-embodiment.”
An April 2022 (12) comprehensive study exploring long-term pain after surgery investigated how pain and function, health-related quality of life, and healthcare resource use evolved over 5 years after total knee replacement. This study focused on those with and without chronic pain 1 year after their primary surgery.
- Chronic pain was reported in 70/552 operated knees (12.7%) 1 year after surgery.
- The chronic pain group had worse pain, function, more hospital readmissions, and health-related quality of life issues pre-surgery and post-surgery as compared to those in the non-chronic pain group. Those without chronic pain markedly improved right after surgery, then plateaued. Those with chronic pain improved slowly but steadily.
- 64.7% of those in chronic pain recovered during the following 4 years, while 30.9% fluctuated in and out of chronic pain.
Urinary incontinence and knee replacement complications
A March 2024 study (13) examined post-operative knee replacement complication risk factors in patients with urinary incontinence. The results of their study suggest patients with incontinence who had primary total knee replacement had higher rates of mechanical failure, aseptic revision, and all-cause revision compared to controls. The study suggests examining the urinary incontinence prior to surgery to decrease the risk factors for knee replacement complication.
Osteoporosis and total knee replacement complication
An April 2024 study (14) looked at the risk osteoporosis may pose in revision surgery of a total knee replacement. The medical records of 41,760 knee replacement patients who had osteoporosis were reviewed for a 5-year incidence of revision surgery to include reasons of periprosthetic fracture, aseptic loosening, and periprosthetic joint infection. Patients who had osteoporosis also had elevated risk of revision surgery for periprosthetic joint infection and aseptic loosening. Complications were seen at higher rate in obese patients.
Post-surgery peripheral nerve injury
An April 2024 paper (15) examined the risk factors for “potentially devastating” peripheral nerve injury following revision total knee replacement. In this study of 132,000 revision total knee replacement patients, doctors found an occurrence rate of 0.56% for post-surgery peripheral nerve injury. Most at risk were in patients with previously diagnosed spine conditions and postoperative anemia.
Post-surgery Covid
An April 2024 paper (16) examined complications in postoperative COVID-19 total knee replacement patients. Patients who contracted Covid-19 within thirty days of total knee replacement had an increased risk of 30-day mortality, infection, pneumonia, ventilator use for more than 48 hours, pulmonary embolism, urinary tract infection, myocardial infarction, deep vein thrombosis, reoperation, readmission, and longer length of hospital stay.
Research: Realistically 9 to 30% of patients do not return to work after knee replacement
In my article: How fast can you get back to work or sport following knee replacement? I refer to studies which suggest that some patients have an over-expectation of what their knee replacement will do for them. Their doctors are concerned that people have a limited understanding of the realistic variables that determine the ability to return to work. In other words – they think they can get back to work sooner than they will actually be able to. As the research of this article shows 9 – 30% of people who have knee replacement, do not return to work.
In my article Do Women Have More Knee Replacement Complications? I discuss research which suggests that in the postoperative period, women, happy that they had the knee replacement lost motivation and confidence in the post-surgery recover. This may help explain, as I cite in the research why women appear to have worse outcomes, more pain, and poorer functional outcomes following total knee replacement than men and what may have caused these outcomes. The research suggests that women had significantly worse pre-surgery pain, limited function, depression, were more likely to be obese, and had pain in more than four joints.
Other factors discussed were knee replacement complications from weak bones in postmenopausal women. The connection of osteoporosis and osteoarthritis commonly coexist in postmenopausal females can be sometimes lost.
Call for a free phone consultation with our staff 800-300-9300
Related video:
Related articles:
Do Women Have More Knee Replacement Complications? Joint Rehab | Los Angeles
Knee replacement outcomes and complications in patients in their 80s and 90s
References
1 Salimy MS, Paschalidis A, Dunahoe JA, Chen AF, Alpaugh K, Bedair HS, Melnic CM. Patients Consistently Report Worse Outcomes Following Revision Total Knee Arthroplasty Compared to Primary Total Knee Arthroplasty. The Journal of Arthroplasty. 2023 Aug 11.
2 Perdisa F, Bordini B, Salerno M, Traina F, Zaffagnini S, Filardo G. Total Knee Arthroplasty (TKA): When Do the Risks of TKA Overcome the Benefits? Double Risk of Failure in Patients up to 65 Years Old. Cartilage. 2023 Apr 19:19476035231164733.
7 Moore A, Eccleston C, Gooberman‐Hill R. “It’s Not My Knee”: Understanding Ongoing Pain and Discomfort After Total Knee Replacement Through Re‐Embodiment. Arthritis care & research. 2022 Jun;74(6):975-81.
8 Zheng H, Shao H, Tang Q, Guo S, Yang D, Zhou Y. Patient-perceived knee enlargement after total knee arthroplasty: prevalence, risk factors, and association with functional outcomes and radiological analysis. International Orthopaedics. 2022 Mar 29:1-8.
9 Zhang JC, Zhang LS, Zhou H, Chen W, Hu ZH, Chen XY, Feng S. Stress distribution patterns during the gait cycle in patients with anterior femoral notching following total knee replacement. BMC Musculoskeletal Disorders. 2022 Dec;23(1):1-8.
10 Lee S, Choi Y, Lee J, Lee H, Yoon J, Chang C. Valgus Arthritic Knee Responds Better to Conservative Treatment than the Varus Arthritic Knee. Medicina. 2023 Apr 17;59(4):779.
11 Zhou L, Dai X, Zhou Z, Kong Q, Duan G, Zhang Y. Effect of total knee arthroplasty for valgus knee correction on clinical outcome and patellar position. International Orthopaedics. 2023 Mar;47(3):735-43.
12 Cole S, Kolovos S, Soni A, Delmestri A, Sanchez-Santos MT, Judge A, Arden NK, Beswick AD, Wylde V, Gooberman-Hill R, Pinedo-Villanueva R. Progression of chronic pain and associated health-related quality of life and healthcare resource use over 5 years after total knee replacement: evidence from a cohort study. BMJ open. 2022 Apr 1;12(4):e058044.
13 Budin JS, Waters TL, Collins LK, Cole MW, Winter JE, Delvadia BP, Iloanya MC, Sherman WF. Incontinence Is an Independent Risk Factor for Total Hip and Knee Arthroplasty. Arthroplasty Today. 2024 Jun 1;27:101355.
14 Harris AB, Lantieri MA, Agarwal AR, Golladay GJ, Thakkar SC. Osteoporosis and Total Knee Arthroplasty: Higher 5-Year Implant-Related Complications. The Journal of arthroplasty. 2023 Oct 30.
15 Chen XT, Korber SS, Gettleman BS, Liu KC, Palmer R, Shahrestani S, Heckmann ND, Christ AB. Risk Factors for Peripheral Nerve Injury Following Revision Total Knee Arthroplasty in 132,960 Patients. The Journal of Arthroplasty. 2024 Apr 1;39(4):1031-5.
16 Wenzel AN, Marrache M, Schmerler J, Kinney J, Khanuja HS, Hegde V. Impact of Postoperative COVID-19 Infection Status on Outcomes in Elective Primary Total Joint Arthroplasty. The Journal of Arthroplasty. 2024 Apr 1;39(4):871-7.
17 Algarni AD. Pes anserinus pain syndrome following total knee arthroplasty for degenerative varus: incidence and predictors. International Orthopaedics. 2020 Jun;44:1083-9.






