Marc Darrow, MD. Joint Rehab Los Angeles
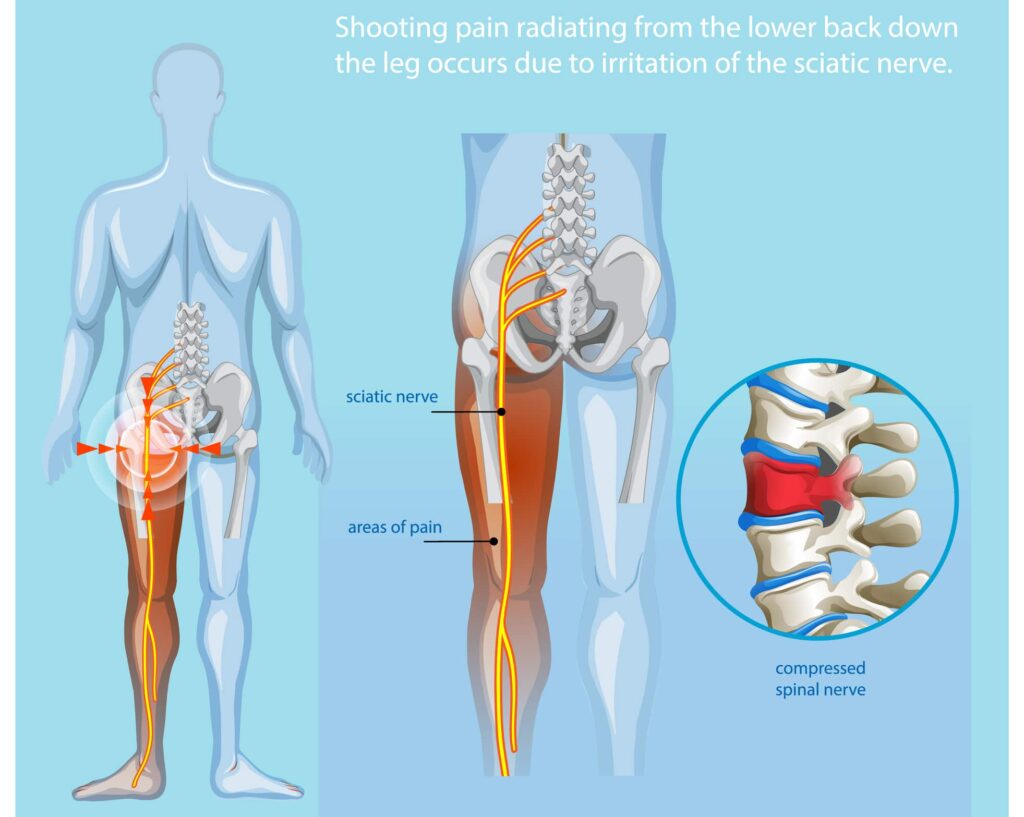
We see many patients diagnosed with sciatica at our Los Angeles joint and spine center. Some, however, come in with a sciatica diagnosis and after physical examination, we discover that they do not have sciatica at all. These new patients may simply have a lumbar sprain or injured ligament. Sciatica is caused by compression of the sciatic nerve by a herniated or bulging disc in the spine. The pain caused by this compression can travel the sciatic nerve all the way, in some instances, down to the feet. A sprained ligament can also mimic this pain. Therefore sciatica can be very difficult to accurately diagnose much less treat.
It is essential to perform a physical examination in suspected cases of sciatica
Above I stated that after a physical examination, we were able to determine that the patient did not have sciatica but another low back issue. It is essential to perform a physical examination in cases of referred pain to isolate the problem as being one where a nerve is being injured or if it is a ligament that is injured.
Often I find that the radiating pain of sciatica is indeed, not because of radiculopathy or pinched nerve, but because of a ligament that is loose or injured because ligaments refer pain the same way. This is why relying on an MRI as the sole diagnostic tool could lead to an unnecessary surgery. If the MRI were to show a degenerative condition, that would be cited as the cause of the radiating pain, even though that may have been a pre-existing condition that caused no pain. A physical examination and conservative treatments will help determine if this is a ligament injury or a nerve compression problem.
Free phone consultation
While sciatica can cause severe pain, conservative care or regenerative medicine can help many people with disability, pain and loss of function.
In our practice, bone marrow aspirate or bone marrow derived Stem Cell Therapy is a treatment for musculoskeletal disorders. We treat degenerative joint disease, degenerative disc disease of the spine, and tendon and ligament injury. With over 27 years of experience, Dr. Marc Darrow and his team are pioneers in regenerative treatments, offering expert insights and personalized care tailored to your needs.
Schedule a free phone consultation today and receive our exclusive Regenerative Medicine Stem Cell & PRP Quick Start Guide —a digital resource packed with:
- Insights into Stem Cell & PRP Therapy
- Research-backed treatments for chronic tendon injuries, joint pain, arthritis, and sports injuries
Take the first step toward a pain-free, active life today.
Call for a free phone consultation with our staff 800-300-9300
More reading
Why treatments for reducing sciatica pain may not work: Joint Rehab Los Angeles






