Patients diagnosed with lumbar spondylolysis and spondylolisthesis are sometimes referred to surgery. The main surgical procedures is spinal fusion, This surgery is designed to stabilize the spine and provide decompression to relieve pressure on the nerves.
In spinal fusion, two vertebrae are joined together, frequently using instrumentation (rods and screws) and bone grafts; in decompression, the bone or tissue that is compressing nerves is removed.
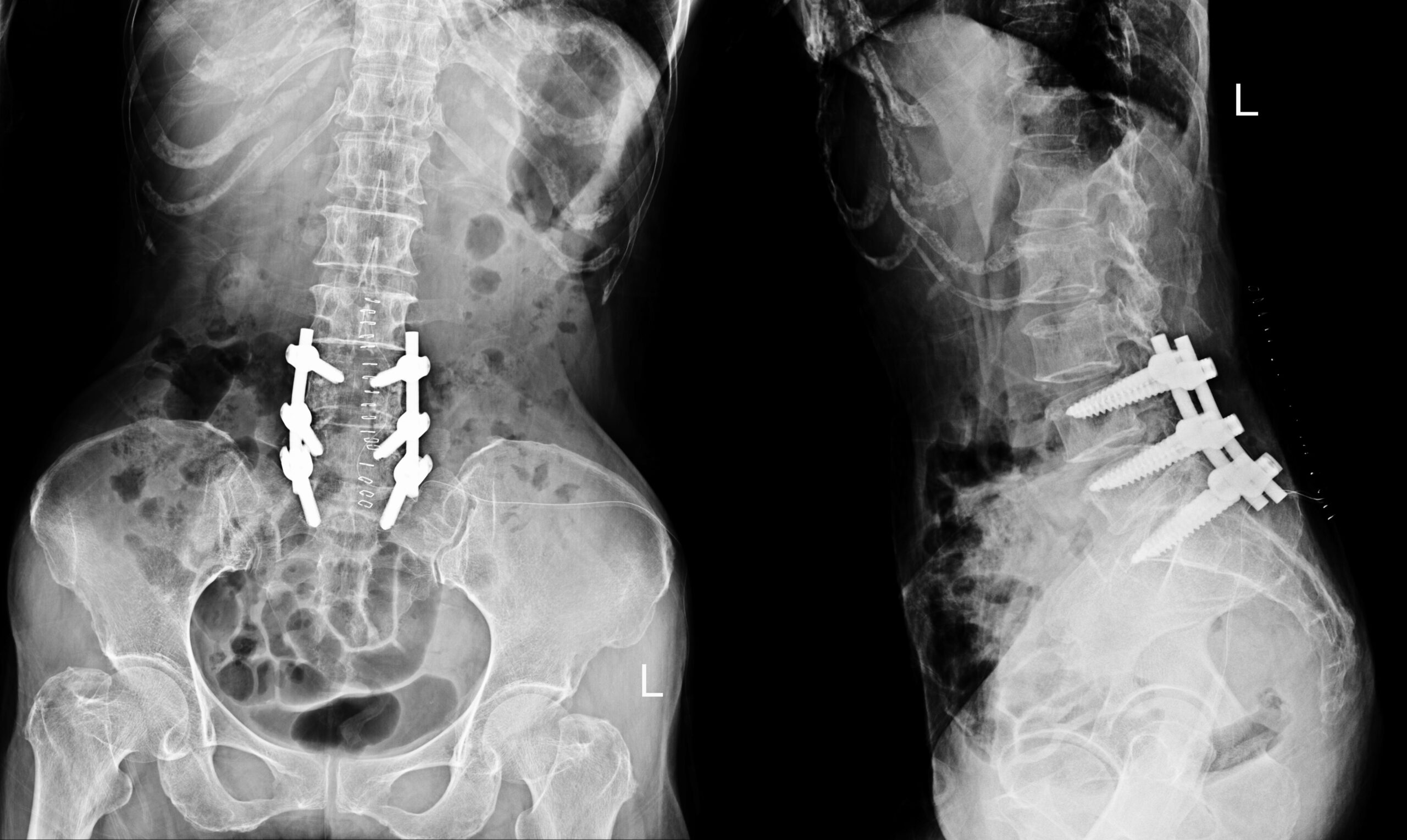
A May 2022 study (1) notes that: “Lumbar spinal fusion surgery is a widely accepted surgical treatment in degenerative causes of lumbar spondylolisthesis. The benefit of reduction (correcting) of anterior displacement (the vertebrae is moving forward over the vertebrae beneath it) and restoration of sagittal parameters (the correct curve of the lumbar spine) is still controversially debated.” Better outcomes, the authors write, can be gained from restoring the lumbar spinal curve.
The fusion of the lumbar spine may lead to the degeneration of the adjacent segments.
An April 2022 study (2) examined the effects of Oblique Lateral Interbody Fusion (OLIF) Surgery (considered less invasive and preserving of more spinal motion after surgery) and TLIF Transforaminal Lumbar Interbody Fusion (TLIF) on adjacent the adjacent spinal segments after treatment of L4 degenerative lumbar spondylolisthesis.
At the last follow-up amongst patients in the two groups, there Adjacent Segment Disease in the OLIF group at 2.78% and 5.56% in the TLIF group. The conclusion of this study was: “L4 degenerative lumbar spondylolisthesis after OLIF and TLIF treatment will cause adjacent segment degeneration, and L3-4 degeneration is more obvious than L5-S1 degeneration. OLIF has more advantages in restoring lumbar sagittal balance (corrected lumbar curve). Compared with TLIF, OLIF can weaken the degeneration of the L5-S1 disc and increase the degeneration of the L5-S1 zygapophyseal joints.
A May 2024 study (3) assessed the appropriateness of surgical decisions in degenerative spondylolisthesis. The authors write: “Selecting patients with lumbar degenerative spondylolisthesis for surgery is difficult. Appropriate use criteria (the research and evidence based decision process in sending a patient or not sending a patient to surgery) have been developed to clarify the indications for lumbar degenerative spondylolisthesis surgery.” The appropriate use criteria however as a tool to understand the appropriateness of surgery in these patients was not able to identify which patients had a greater treatment effect of surgery when compared to non-surgical care. The benefit of surgery relative to non-surgical care was not significantly greater. However, better surgical outcomes were seen in more severe cases.
Free phone consultation
While spondylosis and spondylolisthesis can cause severe pain, conservative care or regenerative medicine can help many people with disability, pain and loss of function.
In our practice, bone marrow aspirate or bone marrow derived Stem Cell Therapy is a treatment for musculoskeletal disorders. We treat degenerative joint disease, degenerative disc disease of the spine, and tendon and ligament injury. With over 27 years of experience, Dr. Marc Darrow and his team are pioneers in regenerative treatments, offering expert insights and personalized care tailored to your needs.
Schedule a free phone consultation today and receive our exclusive Regenerative Medicine Stem Cell & PRP Quick Start Guide —a digital resource packed with:
- Insights into Stem Cell & PRP Therapy
- Research-backed treatments for chronic tendon injuries, joint pain, arthritis, and sports injuries
Take the first step toward a pain-free, active life today.
Call for a free phone consultation with our staff 800-300-9300
Research articles
References
1 Lenz M, Oikonomidis S, Hartwig R, Gramse R, Meyer C, Scheyerer MJ, Hofstetter C, Eysel P, Bredow J. Clinical outcome after lumbar spinal fusion surgery in degenerative spondylolisthesis: a 3-year follow-up. Archives of Orthopaedic and Trauma Surgery. 2020 Dec 29:1-7.
2 Li GQ, Tong T, Wang LF. Comparative analysis of the effects of OLIF and TLIF on adjacent segments after treatment of L4 degenerative lumbar spondylolisthesis. Journal of orthopaedic surgery and research. 2022 Dec;17(1):1-9.
3 Mannion AF, Mariaux F, Werth PM, Pearson AM, Lurie JD, Fekete TF, Kohler M, Haschtmann D, Kleinstueck FS, Jeszenszky D, Loibl M. Evaluation of “appropriate use criteria” for surgical decision-making in lumbar degenerative spondylolisthesis. A controlled, multicentre, prospective observational study. European Spine Journal. 2024 Feb 28:1-3.
584






