We get many emails from people who had a recent MRI. Some of their MRI reports are deep and comprehensive in their description of an unseeingly insurmountable amount of damage to the person’s knees. The person who sends in the email will sometimes add something in the email to suggest that their MRI is one of the worst that their doctor has ever seen. The funny thing is when we ask, “well how does your knee feel today?” Sometimes we get the answer, “not bad.” How can someone who has one of the worst knee MRIs their doctor has ever seen, have a knee that is “not bad”? That is what a lot of research is focusing on. Below we are going to focus on that research that demonstrates that the MRI may not be telling the truth about their pain source, In fact, new findings say that many MRIs are useless.
Research: We should manage the patient, not the MRI or the x-ray
I have been providing regenerative medicine injections for more than 25 years. We always treat the patient. We do not treat the MRI. What does this mean? It means that while the MRI is an important tool in seeing what is going on in the knee, it sometimes shows us too much. It sometimes shows us damage that is not bothering or limiting the patient. If you solely relied on what the MRI is showing and never talked to the patient about how their knee felt, there would be a lot more knee surgeries, and a lot more failed knee surgeries and a lot more people who are worse off. There is a lot of research to back this up.
X-ray reveals the presence of worsening osteoarthritis. Researchers are asking, what should the doctor do next? Get an MRI?
An April 2022 study (1) questioned whether there is a problem of over diagnosis and subsequent overutilization of total knee arthroplasty (replacement). The study noted that medical insurance companies have questions about the over exaggeration of radiographic (MRI) findings and subsequent overutilization of total knee arthroplasty. Currently, the standard of care for assessing potential knee arthroplasty candidates includes assigning a Kellgren-Lawrence (KL) radiographic score. This study investigated the accuracy of reported preoperative Kellgren-Lawrence (KL) radiographic score scores in patients undergoing total knee arthroplasty.
A December 2021 paper (2) assessed the diagnostic accuracy of knee ultrasound for evaluation of meniscus and collateral ligaments pathology in comparison with MRI. The researchers write: “Although magnetic resonance imaging (MRI) is often the “gold standard” for diagnosing knee problems, it has many limitations. Therefore, ultrasonography has been suggested as an effective rapid alternative in many knee abnormalities, especially after injuries of the meniscus and collateral ligaments.”
The researchers found:
- Ultrasound compared to MRI for the assessment and diagnosing of meniscus injuries overall accuracy (91.7% vs. 88.3%).
- Ultrasound compared to MRI for the assessment and diagnosing collateral ligament injures overall accuracy (96.7% vs. 93.3%).
The researchers concluded: “Ultrasonography is a useful screening tool for the initial diagnosis of meniscal and collateral ligament pathology compared to or even with potential advantages over MRI, especially when MRI is unavailable or contraindicated.”
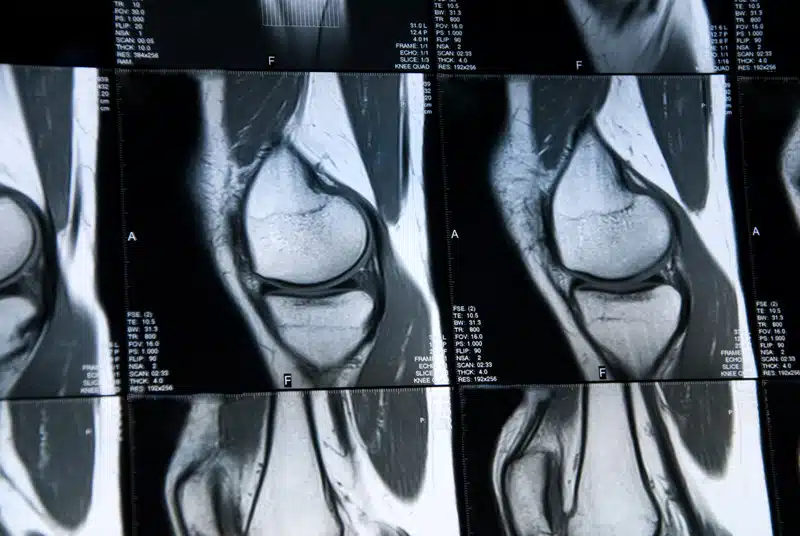
MRI does see cartilage changes
An MRI does see changes to the knee over time. A September 2022 paper (3) investigated the accuracy of MRI in identifying knee cartilage changes over time. The researchers looked at seven previously published studies of 1091 subjects, 355 were males. The results of all the studies, except one, indicated the high accuracy of MRI to identify knee cartilage changes over time. But is it the cartilage changes causing the patient’s pain?
The knee with multiple-ligament injuries
A 2022 paper in the journal BioMed Central musculoskeletal disorders writes: (4) “(this) study found that the accuracy of MRI was good for detecting cruciate ligament injuries, moderate for collateral ligament injuries, low for meniscus injuries. We reviewed the literature and did not find research that investigated the value of MRI in classifying multiple ligament injuries. . . In short, MRI helps early detection of multiple ligament injuries, however, it has limited value in classifying the multiple ligament injuries preoperatively. The management of multiple ligament injuries should be based on comprehensive assessment including preoperative imaging, physical exam, and intraoperative exploration.
Summary
As stated above, I have been providing regenerative medicine injections for more than 20 years. We always treat the patient. We do not treat the MRI. While the MRI is an important tool in seeing what is going on in the knee, it sometimes shows us too much. It sometimes shows us damage that is not bothering or limiting the patient. It may show enough for some to go to a surgery they may not need. If you solely relied on what the MRI is showing and never talked to the patient about how their knee felt, there would be a lot more knee surgeries, and a lot more failed knee surgeries and a lot more people who are worse off.
References
1 Gregory JJ, Ziarati P, Werth PM, Jevsevar DS. Do Physicians Overestimate Radiographic Findings in Patients Undergoing Knee Arthroplasty?. Arthroplasty today. 2022 Jun 1;15:98-101.
2 Elshimy A, Osman AM, Awad ME, Abdel Aziz MM. Diagnostic accuracy of point-of-care knee ultrasound for evaluation of meniscus and collateral ligaments pathology in comparison with MRI. Acta Radiologica. 2021 Dec 1:02841851211058280.
3 Aghdam YH, Moradi A, Großterlinden LG, Jafari MS, Heverhagen JT, Daneshvar K. Accuracy of magnetic resonance imaging in assessing knee cartilage changes over time in patients with osteoarthritis: A systematic review. Northern Clinics of Istanbul. 2022;9(4):414.
4 Li X, Hou Q, Zhan X, Chang L, Ma X, Yuan H. The accuracy of MRI in diagnosing and classifying acute traumatic multiple ligament knee injuries. BMC Musculoskeletal Disorders. 2022 Dec;23(1):1-7.






